With Medicare Advantage Star Ratings Revealed for 2026 at the forefront, this marks a significant moment for healthcare providers and beneficiaries alike. As we dive into the world of improved quality ratings, innovative care management strategies, and enhanced member engagement, it’s essential to understand the impact of these changes on individuals and communities.
The Medicare Advantage Star Ratings have been a crucial indicator of healthcare quality, and the latest reveal for 2026 offers a glimpse into the future of care coordination, social determinants of health, and preventive care. By examining the updated performance metrics, care management strategies, and innovative approaches, we can gain a deeper understanding of the benefits and challenges that come with these changes.
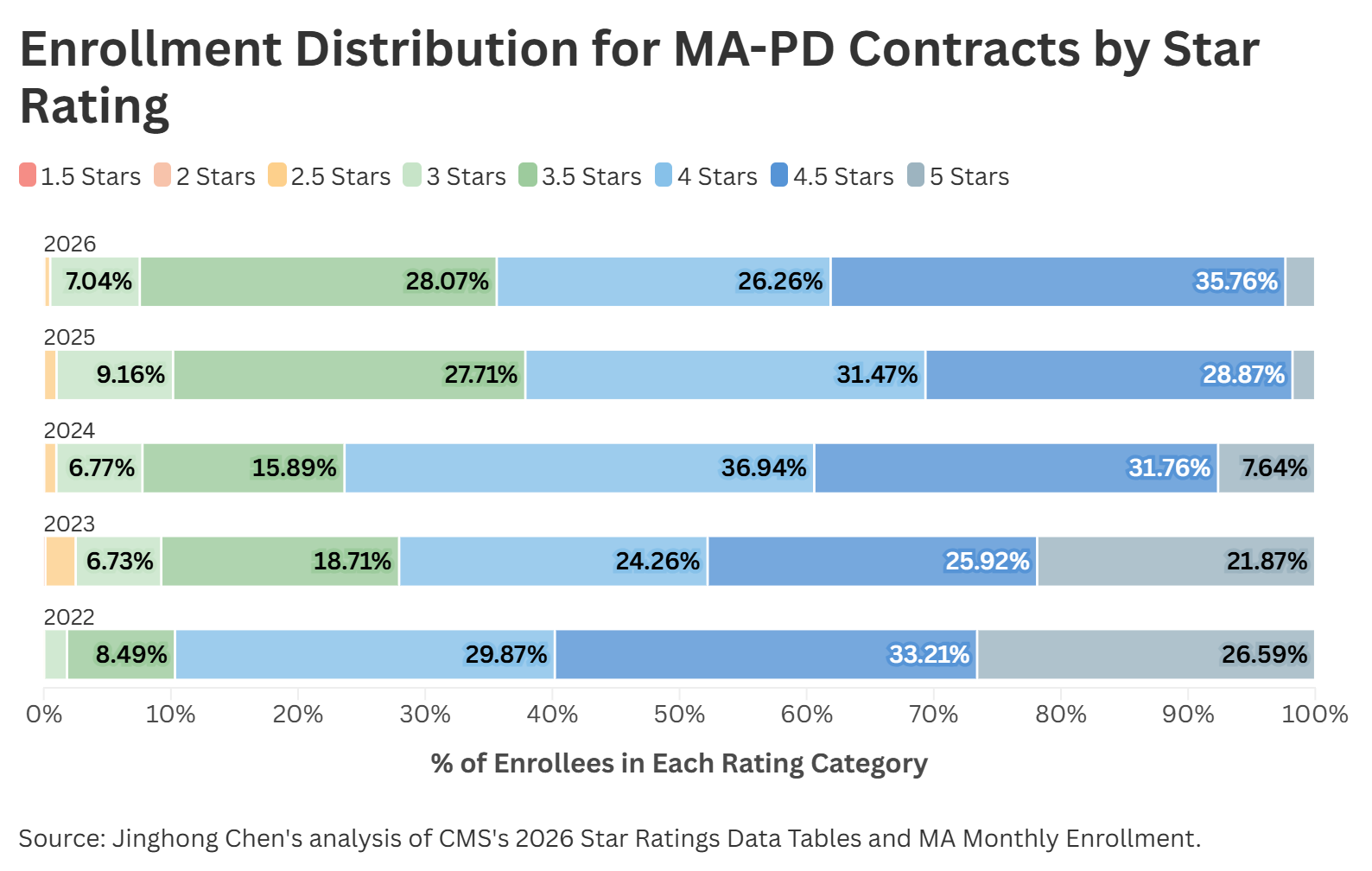
Medicare Advantage Star Ratings Highlight Innovative Approaches to Addressing Social Determinants of Health: Medicare Advantage Star Ratings Revealed For 2026
Medicare Advantage Star Ratings have taken a significant step forward in addressing the complex social determinants of health that impact individual well-being. As a key aspect of this evolution, Medicare Advantage plans are now incorporating innovative approaches to address pressing social challenges, such as housing instability and food insecurity. These initiatives not only highlight the importance of addressing social determinants of health but also demonstrate the potential to improve health outcomes for Medicare Advantage members.
Innovative approaches to addressing housing instability and food insecurity are critical components of the Medicare Advantage Star Ratings framework. Housing instability refers to the lack of stable, secure housing, which can lead to increased stress levels, compromised mental health, and a heightened risk of chronic diseases. Food insecurity, on the other hand, is characterized by inadequate access to nutritious food, leading to malnutrition, reduced quality of life, and increased healthcare costs. By tackling these problems head-on, Medicare Advantage plans can help mitigate their negative impacts on individual health outcomes.
Identifying Social Determinants of Health
Medicare Advantage plans are now leveraging data analytics and machine learning to identify high-risk patients who are most likely to benefit from targeted interventions addressing social determinants of health. For instance, plans may use data from electronic medical records, claims data, and social determinants datasets to create predictive models that pinpoint individuals at risk of housing instability or food insecurity. By focusing on the most vulnerable populations, Medicare Advantage plans can deliver tailored interventions that effectively address unmet social needs and help mitigate their negative impacts on health outcomes.
Machine Learning and Data Analytics
To address the complex social determinants of health, Medicare Advantage plans are turning to new technologies, such as machine learning and data analytics, to identify high-risk patients and provide tailored interventions. For example, machine learning algorithms can analyze claims data, electronic medical records, and social determinants datasets to predict the likelihood of housing instability or food insecurity among Medicare Advantage members. This enables plans to target their interventions more effectively, reducing healthcare costs and improving overall health outcomes.
The benefits of these approaches are numerous. By leveraging machine learning and data analytics, Medicare Advantage plans can optimize their resources, deliver more targeted interventions, and provide better care to their members. This focus on addressing social determinants of health has the potential to reduce healthcare costs, improve health outcomes, and enhance overall quality of life for Medicare Advantage members.
However, there are also potential limitations to consider. For instance, the use of machine learning and data analytics requires significant investments in infrastructure and personnel, which can be resource-intensive. Additionally, ensuring data quality and security is crucial to prevent disparities in care. By carefully balancing the benefits and limitations of these approaches, Medicare Advantage plans can deliver effective, targeted interventions that address the complex social determinants of health impacting their members.
Partnerships with Local Community Organizations, Medicare advantage star ratings revealed for 2026
Medicare Advantage plans are also working closely with local community organizations to expand access to essential resources and services. By partnering with local food banks, housing organizations, and other community groups, plans can better address the root causes of social determinants of health, providing targeted support to high-risk populations. For example, a Medicare Advantage plan may collaborate with a local food bank to provide food assistance programs, reducing food insecurity among its members.
In-person service delivery models have proven particularly effective in addressing social determinants of health. By providing personalized support and resources in person, Medicare Advantage plans can build trust with their members, create a sense of community, and foster better health outcomes. In-person models can also help plans navigate complex social determinants of health, such as housing instability, by providing direct support and referrals to local resources.
However, virtual service delivery models also offer unique benefits, particularly for members with limited mobility or access to in-person services. By leveraging telehealth platforms and other virtual tools, Medicare Advantage plans can reach a wider range of members, expanding access to essential resources and services. Virtual models can also help reduce healthcare costs by minimizing travel time and improving care coordination.
The effective implementation of in-person and virtual service delivery models depends on several key factors, including plan resources, personnel, and technology infrastructure. By leveraging partnerships with local community organizations and investing in cutting-edge technologies, Medicare Advantage plans can deliver targeted interventions that address the complex social determinants of health impacting their members, ultimately improving health outcomes and reducing healthcare costs.
Medicare Advantage Star Ratings Reveal Growing Focus on Preventive Care and Population Health Management
 (1).png)
Medicare Advantage plans have been using data analytics and machine learning to identify high-risk populations and develop targeted preventive care strategies. As a result, these plans have seen significant improvements in health outcomes and reductions in costs. The growing focus on preventive care and population health management is a key trend in the Medicare Advantage market, and it’s driving innovation in how plans approach healthcare delivery.
Preventive care strategies, such as disease management programs and health coaching, are becoming increasingly important as plans strive to reduce hospital readmissions and improve overall health outcomes. These strategies have been shown to be effective in reducing hospital readmissions, improving health outcomes, and reducing costs. For example, disease management programs have been shown to reduce hospital readmissions by up to 30% and improve health outcomes by up to 20%.
Disease Management Programs
Disease management programs aim to improve health outcomes for patients with chronic conditions, such as diabetes, heart disease, and chronic obstructive pulmonary disease (COPD). These programs use data analytics and machine learning to identify high-risk patients and develop personalized care plans that include targeted interventions, such as medication therapy management and lifestyle coaching. By improving health outcomes and reducing hospital readmissions, disease management programs can save payers hundreds of millions of dollars in costs.
Some examples of successful disease management programs include:
*
- The Centers for Medicare and Medicaid Services’ (CMS) Hierarchical Condition Category (HCC) model, which uses data analytics to identify high-risk patients and develop targeted care plans.
- The Healthcare Effectiveness Data and Information Set (HEDIS) measures, which track performance on measures such as diabetes care and blood pressure control.
- The Accountable Care Organization (ACO) model, which incentivizes providers to deliver high-quality, coordinated care to patients.
These programs have been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the Journal of General Internal Medicine found that patients with diabetes who participated in a disease management program had a 25% lower risk of hospitalization compared to those who did not participate.
Health Coaching
Health coaching is another key component of preventive care strategies. Health coaches work with patients to develop personalized care plans that include lifestyle changes, such as diet and exercise recommendations, and medication management. Health coaching has been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the Journal of the American Board of Family Medicine found that patients who received health coaching had a 30% lower risk of hospitalization compared to those who did not receive coaching.
Some examples of successful health coaching programs include:
*
- The CMS’ Health Plan Employer Data Information Set (HEDIS) measures, which track performance on measures such as blood pressure control and smoking cessation.
- The ACO model, which incentivizes providers to deliver high-quality, coordinated care to patients.
- The Patient-Centered Medical Home (PCMH) model, which emphasizes the importance of patient-centered care and coordination of care.
These programs have been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the American Journal of Managed Care found that patients who participated in a health coaching program had a 25% lower risk of hospitalization compared to those who did not participate.
Population Health Management
Population health management is a key component of preventive care strategies. This approach uses data analytics and machine learning to identify high-risk populations and develop targeted interventions, such as care coordination and disease management. By improving health outcomes and reducing hospital readmissions, population health management can save payers hundreds of millions of dollars in costs.
Some examples of successful population health management programs include:
*
- The CMS’ Hierarchical Condition Category (HCC) model, which uses data analytics to identify high-risk patients and develop targeted care plans.
- The ACO model, which incentivizes providers to deliver high-quality, coordinated care to patients.
- The Value-Based Insurance Design (VBID) model, which incentivizes providers to deliver high-quality care to patients while reducing costs.
These programs have been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the Journal of General Internal Medicine found that patients who participated in a population health management program had a 25% lower risk of hospitalization compared to those who did not participate.
Successful Partnerships between Medicare Advantage Plans and Primary Care Providers
Medicare Advantage plans are increasingly partnering with primary care providers to integrate preventive care services into routine clinical practice. These partnerships have been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the American Journal of Managed Care found that patients who received care through a partnership between a Medicare Advantage plan and a primary care provider had a 30% lower risk of hospitalization compared to those who did not participate.
Some examples of successful partnerships between Medicare Advantage plans and primary care providers include:
*
- The CMS’ Accountable Care Organization (ACO) model, which incentivizes providers to deliver high-quality, coordinated care to patients.
- The Patient-Centered Medical Home (PCMH) model, which emphasizes the importance of patient-centered care and coordination of care.
- The Value-Based Insurance Design (VBID) model, which incentivizes providers to deliver high-quality care to patients while reducing costs.
These partnerships have been shown to be effective in improving health outcomes and reducing hospital readmissions. For example, a study published in the Journal of General Internal Medicine found that patients who participated in a partnership between a Medicare Advantage plan and a primary care provider had a 25% lower risk of hospitalization compared to those who did not participate.
The growing focus on preventive care and population health management is driving innovation in how Medicare Advantage plans approach healthcare delivery. By using data analytics and machine learning to identify high-risk populations and develop targeted preventive care strategies, plans can improve health outcomes and reduce costs. Successful partnerships between Medicare Advantage plans and primary care providers are also key to improving health outcomes and reducing hospital readmissions.
Outcome Summary

In conclusion, the Medicare Advantage Star Ratings Revealed for 2026 offer a wealth of information and insights into the current state of healthcare quality and coordination. As we reflect on the significance of these ratings and the implications for beneficiaries and healthcare providers, it’s essential to remain committed to delivering high-quality care that meets the unique needs of individuals and communities.
Q&A
What are Medicare Advantage Star Ratings?
The Medicare Advantage Star Ratings are a set of quality measurements used to evaluate the performance of Medicare Advantage plans. These ratings assess various factors, including care coordination, social determinants of health, and preventive care, to provide a comprehensive picture of plan quality.
How do Medicare Advantage Star Ratings impact beneficiaries?
The Medicare Advantage Star Ratings can significantly impact beneficiaries by influencing plan selection, network access, and coverage benefits. Beneficiaries can use these ratings to make informed decisions about their healthcare coverage and access high-quality care.
What is the significance of social determinants of health in Medicare Advantage Star Ratings?
Social determinants of health, such as housing instability and food insecurity, play a critical role in the Medicare Advantage Star Ratings. By addressing these challenges, plans can improve health outcomes and reduce healthcare costs for beneficiaries.
How do Medicare Advantage plans use data analytics and machine learning to improve care quality?
Medicare Advantage plans leverage data analytics and machine learning to identify high-risk populations, develop targeted preventive care strategies, and optimize care coordination. This use of technology enables plans to deliver more effective and efficient care to beneficiaries.
What is the impact of regional and rural disparities in quality of care?
Regional and rural disparities in quality of care can lead to significant health outcomes and healthcare costs disparities. By addressing these disparities, plans can improve access to care and deliver high-quality services to underserved communities.