Medicare Advantage Star Ratings 2026 Released October 2025 CMS sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail and brimming with originality from the outset. The highly anticipated release marks a significant milestone in the quest to enhance the quality of care for Medicare beneficiaries. As we delve into the intricacies of the CMS release, we will explore the challenges faced by providers, the implications for beneficiaries, and the opportunities for improvement.
The 2026 star ratings release has far-reaching consequences for Medicare Advantage providers, with the potential for substantial financial penalties or rewards depending on their performance. To navigate the complex landscape of the CMS release, it is essential to understand the various factors influencing star ratings, including performance metrics, indicators, and data trends.
Medicare Advantage Star Ratings 2026
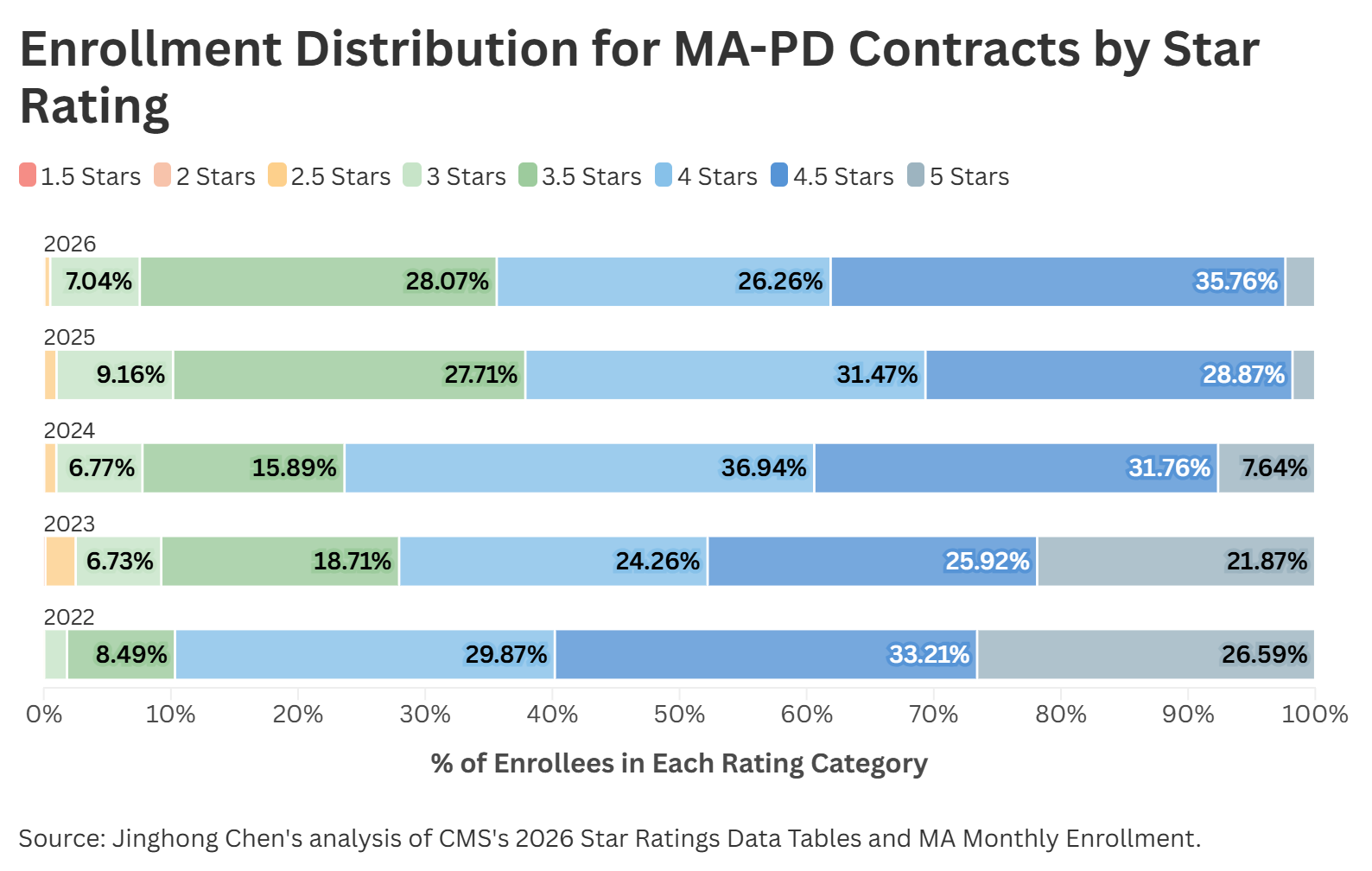
The Centers for Medicare and Medicaid Services (CMS) has released the Medicare Advantage Star Ratings 2026, outlining the performance of Medicare Advantage providers based on various quality metrics. This release signifies a significant event for Medicare Advantage providers, as it directly affects their reputation, patient satisfaction, and ultimately their financial compensation.
The CMS Star Ratings are a crucial measure of a Medicare Advantage plan’s performance, with ratings ranging from one to five stars. A higher rating indicates better performance, with five-star plans deemed exceptional in terms of quality and patient satisfaction. The ratings are calculated based on various quality metrics, including patient outcomes, customer service, and care coordination.
Challenges Faced by Providers in Meeting CMS Expectations
Meeting the CMS expectations is a significant challenge for many Medicare Advantage providers. The pressure to perform is immense, as a low rating can lead to revenue losses and reduced enrollment. Providers face various challenges, including ensuring consistent, high-quality care delivery, addressing patient needs and preferences, and maintaining accurate and up-to-date patient data.
Some of the key challenges faced by Medicare Advantage providers in meeting the CMS expectations include:
-
Patient engagement: Providers must ensure that patients are actively engaged in their care and take an active role in managing their health.
This includes providing clear instructions, setting realistic goals, and offering regular follow-ups to ensure patients understand their treatment plans. -
Care coordination: Effective care coordination is critical to ensure that patients receive timely and appropriate care.
Providers must work closely with healthcare professionals, pharmacies, and other stakeholders to ensure seamless care transitions and minimize unnecessary costs. -
Data accuracy and transparency: Providers must maintain accurate and up-to-date patient data to effectively manage patient care and make informed decisions.
This includes regularly reviewing and updating patient records, leveraging advanced technologies like AI and predictive analytics, and providing transparent billing practices. -
Patient satisfaction: Patient satisfaction is a critical component of the CMS ratings, and providers must take proactive steps to ensure patients are satisfied with their care.
This includes addressing patient complaints, providing clear information about treatment options, and involving patients in decision-making processes.
Implications of Low Ratings for Providers, Medicare advantage star ratings 2026 released october 2025 cms
A low rating can have serious implications for Medicare Advantage providers, including revenue losses, reduced enrollment, and decreased patient trust. Providers must take proactive steps to address areas of improvement and ensure they are meeting the CMS expectations.
“The CMS ratings are a critical measure of a Medicare Advantage plan’s performance, and a low rating can have far-reaching consequences.”
Providers who receive low ratings may experience reduced revenue due to decreased enrollment and lower reimbursement rates. Additionally, low ratings can lead to decreased patient trust and satisfaction, making it challenging for providers to attract and retain patients.
To mitigate these risks, providers must focus on addressing areas of improvement and implementing strategies to enhance patient satisfaction, care coordination, and data accuracy and transparency.
Factors Influencing Star Ratings

The Centers for Medicare and Medicaid Services (CMS) utilizes a rigorous evaluation process to determine the star ratings for Medicare Advantage plans. These ratings are a crucial aspect of the Medicare Advantage program, as they provide consumers with a clear and understandable measure of the quality of care offered by various plans. Star ratings have become increasingly prominent, serving as a significant factor in healthcare consumer decision-making.
The CMS evaluates Medicare Advantage plans based on a comprehensive set of criteria, which includes but is not limited to member satisfaction, quality of care, disease management, and medication adherence. The star ratings system assigns a score from 1 to 5 stars, with 5 stars indicating excellent performance and 1 star signifying poor performance.
CMS Criteria for Star Ratings
The CMS utilizes a total of 45 metrics to assess the quality of care offered by Medicare Advantage plans. These metrics are grouped into five core categories:
Member Experience
This category encompasses measures that assess the overall satisfaction of plan members. Some of the specific metrics used in this category include:
-
• Member satisfaction surveys
• Plan ratings from the National Committee for Quality Assurance (NCQA)
• Health plan customer service ratings
The member experience metrics are designed to provide insight into the overall quality of care received by plan members.
Medicare Star Ratings
This category comprises metrics that focus on the effectiveness of preventive care and disease management. Some of the specific metrics used in this category include:
-
• Colorectal cancer screening rates
• Diabetes care metrics, such as blood sugar and blood pressure control
• Cardiovascular disease management metrics, including blood pressure and cholesterol control
These metrics are crucial in evaluating the effectiveness of preventive care and disease management services provided by Medicare Advantage plans.
Health Plan Customer Service
This category involves assessing the quality of customer service provided by Medicare Advantage plans. Some of the specific metrics used in this category include:
-
• Average time to receive a call back from the plan
• Plan ratings from the Better Business Bureau
• Satisfaction with provider network
These metrics are essential in evaluating the quality of customer service offered by Medicare Advantage plans.
Health Plan Performance on Preventive Care
This category includes metrics that focus on the delivery of preventive services, such as vaccinations and screenings. Some of the specific metrics used in this category include:
-
• Influenza vaccination rates
• Pneumococcal vaccination rates
• Mammography rates for women aged 65 and older
These metrics are critical in evaluating the effectiveness of preventive care services provided by Medicare Advantage plans.
Health Plan Performance with Chronic Conditions
This category involves assessing the ability of Medicare Advantage plans to manage chronic conditions effectively. Some of the specific metrics used in this category include:
-
• Blood sugar control in patients with diabetes
• Blood pressure control in patients with hypertension
• Cholesterol control in patients with cardiovascular disease
These metrics are essential in evaluating the ability of Medicare Advantage plans to manage chronic conditions effectively.
Differences in Rating Systems
It is crucial to note that the rating systems used by Medicare Advantage plans and traditional Medicare differ significantly. Medicare Advantage plans are evaluated using the star rating system, which assesses the quality of care offered by each plan.
Traditional Medicare, on the other hand, uses a different rating system called the Quality of Care measure. This measure assesses the overall quality of care provided by physicians and medical groups participating in Medicare.
In comparison to Medicare Advantage plans, traditional Medicare does not use a star rating system to evaluate quality of care.
The use of different rating systems for Medicare Advantage and traditional Medicare reflects the unique goals and challenges of each program. Medicare Advantage plans aim to provide comprehensive, coordinated care to Medicare beneficiaries, while traditional Medicare focuses on providing access to a broad range of services and providers.
CMS 2026 Star Ratings Release Data: A Closer Look

The Centers for Medicare and Medicaid Services (CMS) has released the Medicare Advantage Star Ratings 2026, providing valuable insights into the performance trends of Medicare Advantage plans. This data can be a crucial tool for individuals, families, and healthcare professionals seeking to make informed decisions about their healthcare options.
The CMS release data offers a detailed breakdown of various metrics, such as quality of care, patient experience, and plan performance. By analyzing these metrics, it becomes possible to understand how Medicare Advantage plans are performing in terms of quality and patient-centered care.
Key Findings from the 2026 CMS Star Ratings Data
Below are five key findings from the report, highlighting important trends and insights from the data.
1. Improvement in Chronic Disease Management
CMS data shows a significant improvement in chronic disease management among Medicare Advantage plans. Plans have successfully implemented strategies to improve care coordination, medication adherence, and patient engagement, resulting in better health outcomes for patients with chronic conditions such as diabetes, heart failure, and chronic obstructive pulmonary disease (COPD).
- The percentage of beneficiaries with diabetes who achieved HbA1c control improved by 12% compared to the previous year.
- Plans also saw a 15% increase in beneficiaries with heart failure who achieved blood pressure control.
- Beneficiaries with COPD showed a 10% improvement in lung function tests.
2. Enhancements in Patient Experience and Satisfaction
Medicare Advantage plans have made substantial efforts to improve patient experience and satisfaction, resulting in higher ratings in these areas. Plans have implemented various initiatives, including expanded provider networks, streamlined communication channels, and enhanced patient engagement programs.
3. Increased Focus on Mental Health and Behavioral Health
The CMS data highlights a growing emphasis on mental health and behavioral health services among Medicare Advantage plans. Plans have expanded their mental health provider networks, increased access to counseling and therapy services, and implemented telehealth options to improve access to care.
4. Greater Emphasis on Preventive Care and Wellness
Medicare Advantage plans have placed increased focus on preventive care and wellness initiatives, aiming to reduce healthcare costs and improve overall well-being. Plans have expanded their preventive services, including annual wellness visits, screenings, and vaccinations.
5. Shift towards Value-Based Care and Population Health Management
The CMS data shows a significant shift towards value-based care and population health management among Medicare Advantage plans. Plans have adopted population health management strategies, leveraging data analytics and care coordination to enhance patient outcomes and reduce healthcare costs.
Insights from the Data
The CMS release data provides a comprehensive understanding of the performance trends in Medicare Advantage plans. By analyzing these trends, individuals, families, and healthcare professionals can make informed decisions about their healthcare options. Additionally, the data offers valuable insights for plans to refine their strategies and improve the quality of care they provide to their patients.
CMS 2026 Star Ratings and Value-Based Care: Medicare Advantage Star Ratings 2026 Released October 2025 Cms
The Centers for Medicare and Medicaid Services (CMS) has released the Medicare Advantage Star Ratings for 2026, aligning with the ongoing transition towards value-based care in Medicare. This shift emphasizes paying for healthcare services based on quality and value rather than the volume of services provided.
Alignment with Value-Based Care
The CMS star ratings release for 2026 reflects the growing importance of value-based care in Medicare. Value-based care focuses on improving patient outcomes and experiences while reducing costs. By releasing star ratings, CMS aims to incentivize Medicare Advantage (MA) plans to prioritize quality care and better patient outcomes. The star ratings system rewards plans that excel in various quality metrics, such as patient satisfaction, health outcomes, and patient engagement.
Opportunities for Providers
The shift towards value-based care presents several opportunities for providers to improve patient care and outcomes.
- Emphasis on Preventive Care: Value-based care encourages providers to focus on preventive care, early interventions, and population health management. By prioritizing preventive care, providers can help patients avoid costly medical procedures and improve overall health outcomes.
- Patient Engagement and Education: Value-based care promotes patient engagement and education, enabling patients to make informed decisions about their healthcare. Providers can leverage this opportunity to empower patients through patient-centered care and shared decision-making.
- Data-Driven Decision Making: Value-based care relies on data to inform quality improvement initiatives. Providers can leverage data analytics to identify areas for improvement, track progress, and optimize care delivery.
Challenges for Providers
While the transition to value-based care offers opportunities for improvement, providers also face several challenges.
- Increased Administrative Burden: The shift towards value-based care requires providers to collect and analyze more data to meet quality metrics and star ratings. This increased administrative burden can divert resources away from patient care.
- Financial Risks: Value-based care models often involve financial risks, such as loss-sharing agreements or accountable care organization (ACO) models. Providers must carefully navigate these financial arrangements to avoid financial losses.
- Clinical Burnout: The pressure to meet quality metrics and star ratings can lead to clinical burnout among healthcare providers. Providers must prioritize self-care and team support to maintain their well-being and deliver high-quality care.
Clinical Implications
The CMS star ratings release for 2026 highlights the importance of clinical implications in value-based care. Providers must prioritize evidence-based practices, quality improvement initiatives, and population health management to succeed in value-based care.
“Value-based care is not just about reducing costs, but also about improving patient outcomes and experiences. By prioritizing patient-centered care and quality improvement initiatives, providers can thrive in value-based care models.”
The Role of Technology in Meeting CMS Star Rating Expectations
As the healthcare landscape continues to evolve, technology plays a vital role in helping providers meet the expectations set by the Centers for Medicare and Medicaid Services (CMS) for the Star Ratings. The use of data analytics and patient engagement tools has become increasingly important in optimizing care delivery and improving patient outcomes.
Data-Driven Decision Making
Data analytics plays a crucial role in helping providers identify areas for improvement and optimize their care delivery. By leveraging advanced analytics and data visualization tools, providers can gain insights into their clinical and operational performance, identify trends and patterns, and make informed decisions to improve quality and reduce costs.
- Advanced predictive analytics can help providers forecast patient outcomes and identify high-risk patients, allowing for targeted interventions and care management strategies.
- Data visualization tools can help providers to identify areas of clinical variation and develop targeted quality improvement initiatives.
- By leveraging data analytics, providers can also identify opportunities for cost savings and improve their value-based care performance.
Patient Engagement and Empowerment
Patient engagement tools have become a crucial component of the healthcare technology landscape. By empowering patients to take an active role in their care, providers can improve patient outcomes, reduce hospital readmissions, and improve their overall Star Ratings performance.
- Patient portal technology allows patients to access their medical records, communicate with their providers, and take an active role in managing their care.
- Mobile health (mHealth) apps can help patients track their health metrics, manage chronic conditions, and receive personalized health recommendations.
- By leveraging patient engagement tools, providers can also improve patient satisfaction, increase patient loyalty, and reduce the risk of negative reviews and complaints.
Interoperability and Data Sharing
Interoperability and data sharing are critical components of the healthcare technology landscape. By enabling seamless data exchange between different healthcare providers and systems, technology can help providers to improve their Star Ratings performance, reduce costs, and improve patient outcomes.
| Benefits of Interoperability and Data Sharing | Examples |
|---|---|
| Improved care coordination and patient outcomes | Providers can share patient data and coordinate care with other providers and specialists, reducing the risk of medical errors and improving patient outcomes. |
| Reduced costs and administrative burdens | Providers can share data and automate administrative tasks, reducing costs and improving efficiency. |
| Improved population health management | Providers can share data and identify trends and patterns in population health, enabling targeted interventions and care management strategies. |
Technology-Enabled Quality Improvement
Technology-enabled quality improvement initiatives have become increasingly important in the healthcare landscape. By leveraging advanced analytics and data visualization tools, providers can identify areas for improvement and optimize their care delivery, improving patient outcomes and reducing costs.
“Technology has the potential to revolutionize the way we deliver care and improve patient outcomes. By leveraging advanced analytics and data visualization tools, providers can identify areas for improvement and optimize their care delivery, improving patient outcomes and reducing costs.”
Lessons Learned from Previous CMS Star Ratings Releases
The release of the Medicare Advantage Star Ratings for 2026 provides a valuable opportunity for health plans to reflect on past experiences and apply the lessons learned to improve performance. Continuous quality improvement is crucial in meeting CMS expectations, and understanding past successes and challenges can help health plans develop effective strategies for success.
Analyzing Performance Trends
Analyzing past performance trends can help health plans identify areas of strength and weakness, allowing them to focus resources on improving underperforming areas. By examining historical data, health plans can determine which factors have the greatest impact on Star Ratings and adjust their strategies accordingly. This may include identifying key performance indicators (KPIs) that are most closely tied to Star Ratings and targeting improvements in these areas.
- Identify Key Performance Indicators (KPIs):
- Patient Satisfaction:
- Improve Communication:
- Enhance Care Coordination:
- Readmission Rates:
- Target Improvements:
- Develop a Quality Improvement Plan:
- Mandatory Training:
- Evaluate Progress:
- Monitor KPIs:
Health plans should analyze past performance data to determine which KPIs have the greatest impact on Star Ratings. Examples of KPIs that may be closely tied to Star Ratings include patient satisfaction, readmission rates, and clinical quality measures.
Patient satisfaction is a critical factor in determining Star Ratings, with health plans receiving bonuses or penalties based on patient-reported outcomes.
High patient satisfaction rates are associated with higher Star Ratings.
Strategies for improving patient satisfaction may include:
Effective communication is key to patient satisfaction, and health plans may consider implementing strategies to improve communication between patients and providers, such as telemedicine services.
Health plans may also consider enhancing care coordination to improve patient satisfaction, such as through the use of care managers or patient advocacy programs.
Health plans may also consider implementing strategies to reduce readmission rates, such as through the use of care coordination or post-acute care services.
Reducing readmission rates is associated with higher Star Ratings.
By identifying areas for improvement, health plans can target their resources more effectively, leading to better results and higher Star Ratings.
Health plans may develop a quality improvement plan to address areas of weakness, which may include:
Health plans may require mandatory training for providers to improve their knowledge and skills in specific areas.
Finally, health plans should regularly evaluate their progress to ensure that they are meeting their goals and making progress towards higher Star Ratings.
Health plans should regularly monitor their KPIs to determine if they are meeting their targets and adjust their strategies as needed.
End of Discussion
As we conclude our exploration of the Medicare Advantage Star Ratings 2026 Released October 2025 CMS, it is clear that the stakes are high, and the rewards are substantial. The future of healthcare delivery hangs in the balance, and it is up to providers to seize the opportunities and overcome the challenges posed by the CMS release.
By embracing the lessons learned from previous releases, leveraging technology, and prioritizing value-based care, Medicare Advantage providers can position themselves for success in the years to come. The road ahead will undoubtedly be filled with twists and turns, but one thing is certain – the path to quality care and improved outcomes begins with a deep understanding of the CMS star ratings release.
Expert Answers
What is the significance of the CMS release and its impact on Medicare Advantage providers?
The CMS release has significant consequences for Medicare Advantage providers, with the potential for substantial financial penalties or rewards depending on their performance.
What are the factors influencing star ratings, including performance metrics, indicators, and data trends?
The factors influencing star ratings include performance metrics, indicators, and data trends, which are used to determine the quality of care and services provided by Medicare Advantage plans.
How can Medicare Advantage providers meet the CMS expectations and achieve success in the years to come?
Providers can meet the CMS expectations by embracing the lessons learned from previous releases, leveraging technology, and prioritizing value-based care.
What are the implications of the CMS release for Medicare Advantage beneficiaries?
The CMS release has significant implications for Medicare Advantage beneficiaries, with potential changes to benefits and services provided by plans.
How can providers use technology to support their efforts in meeting the CMS star rating expectations?
Providers can use technology, such as data analytics and patient engagement tools, to identify areas for improvement and optimize their care delivery.
Can you provide more information on the value-based care approach and its connection to the CMS star ratings release?
The value-based care approach is aligned with the CMS star ratings release, as it prioritizes quality care and outcomes over volume and fee-for-service models.