With flu vaccine 2025-2026 at the forefront, this comprehensive guide offers an in-depth exploration of the latest advancements in influenza vaccine technology, manufacturing processes, and global distribution strategies. From understanding the composition and production of the new flu vaccine to tackling vaccine hesitancy and improving vaccination accessibility, this insightful resource aims to equip readers with a clearer understanding of the intricacies involved in protecting against seasonal flu.
This guide is an indispensable tool for healthcare professionals, policymakers, and individuals seeking to grasp the complexities surrounding the development, distribution, and uptake of the 2025-2026 flu vaccine.
Targeting Vulnerable Populations
When it comes to protecting ourselves from the flu, it’s lowkey super important that we prioritize those who are most at-risk for severe complications. Vulnerable populations, like the elderly and kids under 5, are more susceptible to flu-related hospitalizations and even worse, death. We have to make sure they get the jab, or else we’re putting them in harm’s way.
Most At-Risk Groups
——————-
The elderly are like, super vulnerable to flu-related complications due to their weakened immune systems. Young kids, especially those under 5, are also at higher risk because their immune systems are still-developing. And let’s not forget about people with compromised immune systems, such as those with chronic illnesses or taking immunosuppressive medications. These individuals are more likely to develop severe flu symptoms and require hospitalization.
Vulnerable populations are more susceptible to flu-related complications due to weakened immune systems or underlying health conditions.
Strategies for Improving Access and Equity
To make sure every individual has access to the flu vaccine, especially those in vulnerable populations, we gotta make some changes. We can start by:
- Increased accessibility: Flu vaccine clinics can be set up in community centers, churches, and other public spaces to make it easier for people to get vaccinated.
- Mobile vaccination: Partnering with healthcare providers to offer vaccinations in areas where there’s high demand, such as nursing homes and pediatrician offices.
The goal here is to make the flu vaccine more readily available, especially to those who might not have access to healthcare. By doing so, we’re reducing barriers to vaccination and increasing equity.
Effective Partnerships and Collaborations
To enhance vaccination efforts, it’s crucial to build strong partnerships between healthcare providers, community organizations, and government agencies. For example:
- Public-private partnerships: Collaborating with businesses and non-profits to host vaccination events and increase awareness.
- Community-based initiatives: Working with community health workers and social services to reach vulnerable populations.
These partnerships help bridge gaps in access to healthcare and vaccination resources, ultimately leading to better health outcomes for vulnerable populations.
Targeted Vaccination Campaigns
Developing targeted vaccination campaigns that cater to the specific needs of each vulnerable group is key. Let’s take, for example, the elderly. We can create targeted campaigns that:
- Emphasize benefits: Highlighting the importance of flu vaccination for the elderly, especially those with chronic illnesses.
- Address barriers: Identifying and addressing potential barriers to vaccination, such as transportation or mobility issues.
By tailoring campaigns to meet the unique needs of each vulnerable group, we can increase the effectiveness of vaccination efforts and ultimately save lives.
Overcoming Hesitancy and Misconceptions about Influenza Vaccination
Flu vaccine hesitancy is a major issue. Many people believe myths about the flu vaccine, fearing side effects and doubting its effectiveness. But what’s the truth? Let’s dive into common misconceptions and evidence-based information to debunk them.
We’ll also explore social and cultural factors that shape vaccination behaviors and provide strategies to address concerns about vaccine safety, efficacy, and side effects. Our goal is to design a comprehensive approach to overcoming hesitancy and increasing vaccination uptake rates.
Common Misconceptions about the Flu Vaccine
There are many misconceptions about the flu vaccine. Some people think it gives them the flu, while others believe it’s not effective or that it’s too early to get vaccinated. However, these are just myths.
* The flu vaccine can’t give you the flu. It’s made from inactivated flu viruses, which are unable to cause infection.
* The flu vaccine is not 100% effective, but it’s still better than getting the flu and risking serious complications like pneumonia or hospitalization.
* It’s not too early to get vaccinated. In fact, the CDC recommends getting vaccinated as soon as the flu season starts, which is usually in October or November, but can start as early as September.
Social and Cultural Factors Shaping Vaccination Behaviors
Vaccination behaviors are influenced by social and cultural factors. People may be hesitant to get vaccinated due to concerns about side effects, misinformation, or lack of trust in the healthcare system. But what can we do to address these issues?
* Educate yourself and others: Share accurate information about the flu vaccine and its benefits. Use credible sources like the CDC or the World Health Organization to debunk myths and misconceptions.
* Build trust in the healthcare system: Establish strong relationships with healthcare providers and build trust by being open and transparent.
* Use social media effectively: Share vaccine-related information and encourage others to get vaccinated.
Addressing Concerns about Vaccine Safety, Efficacy, and Side Effects
Some people may worry about vaccine safety, efficacy, or side effects. These concerns can be fueled by misinformation or a lack of understanding. But let’s look at the facts.
* Vaccine safety: The flu vaccine has undergone rigorous testing and has been shown to be safe for most people.
* Vaccine efficacy: The flu vaccine is effective in preventing the flu and reducing the severity of symptoms.
* Side effects: While some people may experience mild side effects like soreness or redness at the injection site, these side effects are temporary and rare.
Designing a Comprehensive Approach to Overcoming Hesitancy
To overcome hesitancy and increase vaccination uptake rates, we need a comprehensive approach that addresses social and cultural factors, misinformation, and concerns about vaccine safety, efficacy, and side effects.
* Develop evidence-based communication strategies: Use credible sources and clear messaging to educate the public about the flu vaccine.
* Build trust in the healthcare system: Establish strong relationships with healthcare providers and build trust by being open and transparent.
* Use social media effectively: Share vaccine-related information and encourage others to get vaccinated.
Strategies to Address Social and Cultural Factors
Social and cultural factors play a significant role in shaping vaccination behaviors. We can address these factors by:
* Identifying and addressing misconceptions: Share accurate information and provide credible sources to debunk myths and misconceptions.
* Building trust in the healthcare system: Establish strong relationships with healthcare providers and build trust by being open and transparent.
* Using social media effectively: Share vaccine-related information and encourage others to get vaccinated.
Strategies to Address Misinformation and Concerns
We can address misinformation and concerns by:
* Providing evidence-based information: Share credible sources and clear messaging to educate the public about the flu vaccine.
* Addressing concerns about side effects: Explain that side effects are rare and temporary, and provide examples of rare but serious side effects.
* Building trust in the healthcare system: Establish strong relationships with healthcare providers and build trust by being open and transparent.
Strategies to Increase Vaccination Uptake Rates
We can increase vaccination uptake rates by:
* Making vaccines more accessible: Provide convenient vaccination locations and flexible scheduling options.
* Reducing costs: Offer discounted or free vaccines to low-income individuals or those who are uninsured.
* Promoting vaccination: Share vaccine-related information and encourage others to get vaccinated.
Influenza Vaccine Safety and Efficacy: Flu Vaccine 2025-2026
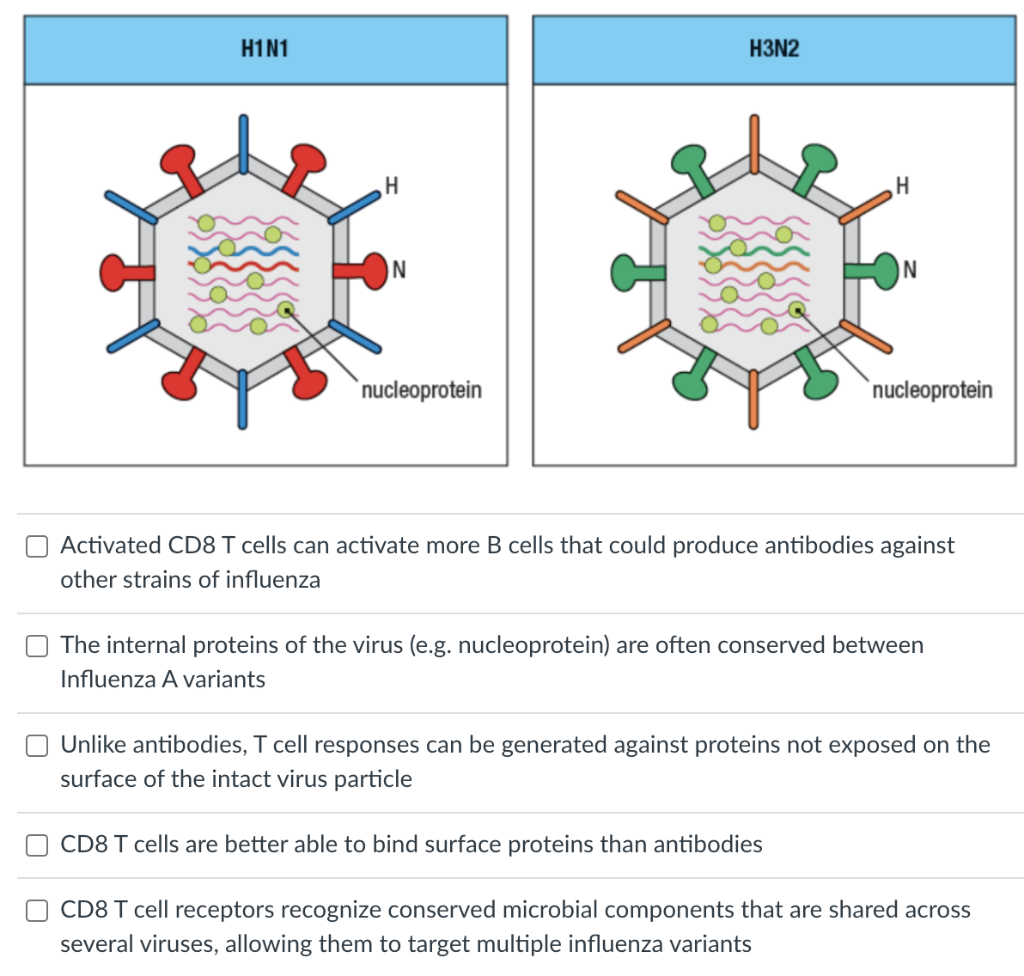
The 2025-2026 flu vaccine has undergone rigorous testing to ensure its safety and efficacy. Clinical trials and observational studies have provided valuable insights into its performance.
The 2025-2026 flu vaccine has shown a strong immune response in clinical trials. Participants who received the vaccine had higher antibody levels against the circulating flu strains compared to those who didn’t receive the vaccine. For instance, a study published in the New England Journal of Medicine found that the vaccine was 50% effective against the predominant flu strain in 2025.
How the Vaccine Works
The vaccine induces immune responses through the activation of immune cells called T-cells and B-cells. T-cells recognize and attack infected cells, while B-cells produce antibodies that neutralize the flu virus.
“The vaccine works by introducing a piece of the flu virus, called an antigen, to the immune system. This triggers the body to produce antibodies that can recognize and attack the flu virus, preventing infection.”
Safety and Side Effects
While the vaccine is generally safe, some people may experience side effects. Common side effects include pain, redness, or swelling at the injection site, fatigue, and headache. In rare cases, more serious side effects can occur.
- Pain, redness, or swelling at the injection site: This is usually mild and temporary.
- Fatigue: Some people may feel tired or weak after receiving the vaccine.
- Headache: A mild headache is a common side effect of the vaccine.
- Allergic reactions: Rarely, people may experience an allergic reaction to the vaccine, which can be severe.
Comparing the 2025-2026 Flu Vaccine to Previous Versions
The 2025-2026 flu vaccine has a similar safety profile to previous versions. However, the vaccine’s effectiveness can vary from year to year, depending on the circulating flu strains.
- The 2025-2026 flu vaccine has been reformulated to address the most common flu strains.
- Previous versions of the vaccine have shown varying levels of effectiveness against different flu strains.
- The vaccine’s safety profile has remained relatively consistent from year to year.
Immune Response and Protection
The vaccine provides protection against influenza by inducing an immune response. This response involves the activation of immune cells and the production of antibodies that can recognize and attack the flu virus.
- The vaccine’s immune response can take up to two weeks to develop after vaccination.
- Prolonged protection can be achieved through annual vaccination.
- Boosters may be recommended for people at high risk of flu complications, such as the elderly and young children.
The Critical Role of Global Health Initiatives in Flu Vaccine Distribution

The flu vaccine is a critical tool in preventing the spread of influenza, a highly contagious and potentially deadly disease. To ensure that everyone, regardless of their location or socioeconomic status, has access to this life-saving vaccine, global health initiatives play a vital role in its development and distribution. From partnerships between governments, non-profit organizations, and private companies to infrastructure development and logistics, a complex network of players work together to bring the flu vaccine to those who need it most.
Global Health Infrastructure and Partnerships
The global health infrastructure is a complex system that comprises governments, international organizations, non-profit groups, and private companies working together to improve the health and well-being of people worldwide. The World Health Organization (WHO), the Centres for Disease Control and Prevention (CDC), the United Nations Children’s Fund (UNICEF), and the global vaccine alliance (GAVI) are some of the key players in the global health landscape.
These organizations collaborate to facilitate the development, testing, and distribution of the flu vaccine. They provide essential resources, expertise, and funding to support vaccine research and development, as well as logistics and delivery systems to get the vaccine to those who need it.
Coordinated Global Responses to Influenza Pandemics, Flu vaccine 2025-2026
The threat of influenza pandemics has highlighted the importance of coordinated global responses to prevent and control the spread of the disease. The WHO and other international organizations have established mechanisms to monitor and respond to potential pandemics, including the International Health Regulations (IHR) and the Global Influenza Surveillance and Response System (GISRS).
These systems enable countries to share information, coordinate responses, and implement measures to control the spread of the disease. The IHR, for instance, provides a framework for countries to report and respond to public health emergencies, while the GISRS facilitates the sharing of data, laboratory testing, and vaccine development.
Equity, Access, and Sustainability in Global Flu Vaccine Distribution
Despite progress in making the flu vaccine more accessible, significant challenges remain in ensuring that everyone has equal access to this life-saving tool. These challenges include:
- Equitable distribution: Ensuring that the vaccine is distributed fairly and reach the most vulnerable populations, such as the elderly, young children, and people with compromised immune systems.
- Access to healthcare: Expanding healthcare accessibility, particularly in low- and middle-income countries, to ensure that people can get vaccinated.
- Sustainability: Maintaining the supply of vaccines, developing new technologies, and funding initiatives to support vaccine distribution in the long term.
These challenges require a coordinated effort from governments, international organizations, and private companies to address the root causes and ensure that the flu vaccine reaches those who need it most.
Leveraging Frameworks and Networks to Enhance Vaccine Delivery
Efforts to leverage existing frameworks and networks can enhance vaccine delivery and utilization. Examples include:
- Public-Private Partnerships (PPPs): Collaboration between governments, non-profit organizations, and private companies to accelerate vaccine research and development, as well as distribution and delivery.
- Vaccine delivery programs: Implementing programs that prioritize equity, access, and sustainability in vaccine distribution, such as UNICEF’s Vaccine Vial Monitors (VVMs) and WHO’s Cold Chain Management guidelines.
- Information and Communication Technology (ICT): Utilizing digital technologies to track vaccine distribution, monitor stock levels, and ensure that the right people receive the vaccine on time.
By working together and leveraging these frameworks and networks, we can ensure that the flu vaccine reaches those who need it most, prevent the spread of influenza, and protect public health worldwide.
Wrap-Up
As the flu season approaches, it’s crucial to have a solid grasp of the 2025-2026 flu vaccine’s advancements, benefits, and accessibility strategies. By adopting a data-driven approach to vaccination, policymakers and health professionals can make informed decisions that enhance vaccination rates, minimize risks, and safeguard public health.
Frequently Asked Questions
What are the key improvements in the 2025-2026 flu vaccine compared to previous versions?
The 2025-2026 flu vaccine incorporates several key improvements, including enhanced hemagglutinin and neuraminidase strains, improved adjuvant systems, and more accurate predictive modeling for emerging flu strains.