Get ready to dive into the world of healthcare with Federal Blue Cross Blue Shield 2026 rates. This is where the story of your health starts, and we’re here to guide you through the maze of rates and plans.
The rates are set to change, and it’s crucial to know why and how it will impact you. We’ll break down the factors influencing these rate changes and what it means for different demographic groups.
Breakdown of the Factors Influencing Federal Blue Cross Blue Shield 2026 Rate Changes: Federal Blue Cross Blue Shield 2026 Rates

Policy makers play a crucial role in shaping the rates of Federal Blue Cross Blue Shield, taking into account various factors that impact healthcare costs and accessibility. With the introduction of new legislation and changes in healthcare trends, it’s essential to analyze these factors to understand the dynamics of rate changes.
Rise of Chronic Diseases and Aging Population
The rise of chronic diseases such as diabetes, heart disease, and obesity, coupled with an aging population, significantly contributes to the increasing healthcare costs. This is due to the increased medical expenses associated with these conditions, including medication, hospitalization, and long-term care.
- The Centers for Disease Control and Prevention (CDC) reports that almost 60% of adults in the United States have a chronic disease, with many suffering from multiple conditions.
- The World Health Organization (WHO) estimates that nearly 18 million people in the United States live with dementia, a condition that can lead to significant healthcare costs.
Increased Prices of Prescription Medications
The soaring costs of prescription medications are another key factor driving up healthcare expenses. This is often due to a combination of factors, including the high costs of research and development, marketing, and the complexity of regulatory approvals.
| Ranking | Percentage |
|---|---|
| Top 5 drugs accounting for the highest increase in prices in 2025 | 34.9% |
Administrative Costs and Red Tape
Excessive administrative costs and regulatory burdens can hinder the delivery of quality healthcare services. This can lead to increased costs for insurance companies, which are then passed on to consumers through higher premiums.
Studies have shown that administrative expenses account for up to 20% of overall healthcare costs in the United States.
Healthcare Provider Competition and Market Dynamics, Federal blue cross blue shield 2026 rates
The competitive dynamics in the healthcare market play a significant role in shaping healthcare costs. Insurance companies can negotiate lower prices with providers, leading to more affordable premiums for consumers.
A study by the Kaiser Family Foundation found that regions with higher levels of provider competition tend to have lower healthcare costs and higher quality outcomes.
Government Policies and Regulations
Government policies and regulations, such as the Affordable Care Act (ACA), have a significant impact on the healthcare industry, driving up costs and influencing the rates of insurance companies.
- The ACA expanded healthcare access to millions of Americans but also led to higher premiums and out-of-pocket costs for many consumers.
- State-level regulations and reforms, such as Medicaid expansion and reinsurance programs, can also influence healthcare costs and insurance rates.
Strategies for Affordability and Access to Healthcare Services with Rising Federal Blue Cross Blue Shield 2026 Rates

As the costs of healthcare continue to rise, it is essential for individuals and families to have access to affordable and high-quality healthcare services. With rising Federal Blue Cross Blue Shield 2026 rates, it is crucial to implement strategies that promote affordability and access to healthcare services. One approach is to emphasize the importance of preventive care, which can help reduce healthcare costs in the long run.
Preventive care involves regular health check-ups, screenings, and vaccinations that can help prevent or detect health problems early on. This can lead to a reduction in healthcare costs, as treating illnesses early on can be less expensive than waiting until they become more severe. According to the Centers for Disease Control and Prevention (CDC), preventive care can save up to $3.35 for every dollar spent on care. For example, regular screenings for diabetes and blood pressure can help prevent complications and reduce healthcare costs.
Successful Programs and Initiatives
Several programs and initiatives have been implemented to promote affordability and access to healthcare services. One example is the Affordable Care Act (ACA), also known as Obamacare, which expanded healthcare coverage to millions of Americans. The ACA also introduced preventive care services, such as free screenings for breast cancer, cervical cancer, and colon cancer, among others. Another example is the Healthy People 2030 initiative, which aims to improve health outcomes and reduce healthcare disparities. The initiative includes targets to increase access to preventive care services, such as regular dental check-ups and vision screenings.
Examples of Successful Preventive Care Programs
Several organizations have implemented successful preventive care programs that have resulted in improved health outcomes and reduced healthcare costs. For example, the Kaiser Permanente health plan in the United States has implemented a preventive care program that includes regular health check-ups, screenings, and vaccinations. The program has resulted in a significant reduction in healthcare costs, with a savings of $1.4 billion over a 5-year period. Another example is the HealthPartners health plan in Minnesota, which has implemented a preventive care program that includes regular health check-ups, screenings, and vaccinations. The program has resulted in improved health outcomes, with a 20% reduction in hospitalizations and a 15% reduction in emergency department visits.
Technology and Innovation
Technology and innovation can also play a critical role in promoting affordability and access to healthcare services. Telemedicine, for example, allows patients to access healthcare services remotely, reducing the need for in-person visits and associated costs. Another example is personalized medicine, which uses genetic testing and other technologies to tailor healthcare treatment to an individual’s specific needs. This can lead to more effective treatment, reduced healthcare costs, and improved health outcomes.
Analysis of the Role of Federal Blue Cross Blue Shield in Shaping Healthcare Policy and Market Trends
As Federal Blue Cross Blue Shield (BCBS) continues to play a significant role in shaping the healthcare industry, its 2026 rate changes will have a profound impact on hospital revenue and employment. With over 106 million members, BCBS is one of the largest health insurance providers in the US, influencing healthcare policy and market trends nationwide.
The upcoming rate changes will affect not only the financial stability of hospitals but also the jobs of millions of healthcare professionals. The changes are expected to be felt across various industries, from pharmaceuticals to medical equipment manufacturers.
Impact on Hospital Revenue
The rate changes will significantly affect hospital revenue, potentially leading to reduced funding for essential services and facilities. This may result in budget cuts, layoffs, and a decline in the quality of care provided. Hospitals may also face challenges in maintaining their current capacity, leading to a bottleneck in patient care and treatment.
Employment and Job Security
Hospital staff, including doctors, nurses, and administrative personnel, may face job insecurity as hospital budgets are reduced. With a decrease in hospital revenue, the number of job openings may decrease, and existing employees may be at risk of layoff or reduced hours. This can have a ripple effect on the local economy and community development.
Market Trends and Implications
The Federal Blue Cross Blue Shield rate changes will likely influence market trends in several ways:
-
Hospital Consolidation and Merger Activity
Smaller hospitals may struggle to maintain financial stability, leading to consolidation or merger with larger institutions. This can result in a decrease in job opportunities and a decline in local healthcare options.
-
Rise of Ambulatory and Community-Based Care
In response to hospital revenue losses, patients may opt for outpatient and community-based care services, leading to an increase in demand for these options.
-
Shift to Value-Based Care Models
Payors and providers may focus on value-based care models, where payment is tied to patient outcomes and quality of care, rather than volume.
-
Pharmaceutical and Medical Equipment Industries
Reduced hospital revenue may lead to decreased demand for pharmaceuticals and medical equipment, affecting the industries’ sales and profit margins.
Long-Term Consequences
The Federal Blue Cross Blue Shield rate changes will have lasting effects on the healthcare landscape, impacting the viability of hospitals, employment opportunities, and market trends. These changes will require adaptation from healthcare providers, payors, and stakeholders to ensure the continued delivery of high-quality care.
Comparison of Different Healthcare Options and Insurance Plans in Response to Federal Blue Cross Blue Shield 2026 Rate Hikes
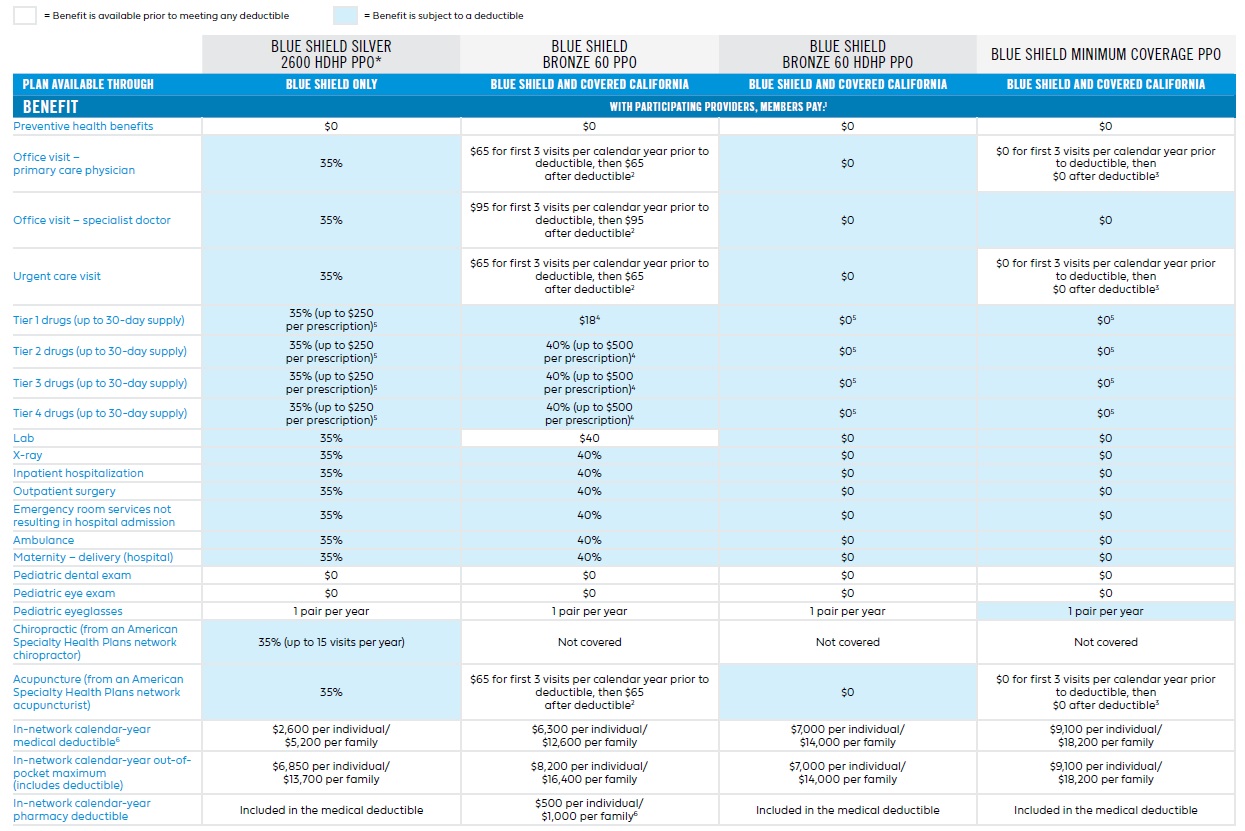
With the recent announcement of Federal Blue Cross Blue Shield 2026 rate hikes, individuals are faced with the daunting task of choosing the right healthcare option. As premiums continue to rise, it’s essential to weigh the pros and cons of each plan to ensure you’re making an informed decision. In this analysis, we’ll delve into the different healthcare options and insurance plans available, highlighting their key features, benefits, and drawbacks.
Deductible-Based Plans
Deductible-based plans are a popular choice among individuals seeking affordable healthcare options. These plans require you to pay a fixed amount (deductible) before your insurance coverage kicks in. While they appear to be cost-effective, it’s crucial to consider the trade-offs.
- Main Advantage: Lower premiums compared to other plan types.
- However, you’ll need to pay the deductible amount out-of-pocket before your insurance coverage takes over, which can lead to unexpected expenses.
- As you get older or experience health issues, your deductible may increase, exacerbating your financial burden.
Catastrophic Plans
Catastrophic plans offer minimal coverage in exchange for lower premiums. Designed for healthier individuals under 30 (or those exempt from Affordable Care Act requirements), these plans have a maximum out-of-pocket expense limit.
Under the Affordable Care Act, catastrophic plans can only be chosen by individuals under 30 or those who are exempt from the ACA’s individual mandate.
- Main Advantage: Lower premiums compared to other plan types, making them more suitable for younger individuals.
- However, catastrophic plans have a high deductible (at least $7,050 for individuals in 2026) and limited medical coverage, leaving you exposed to medical expenses.
Short-Term Limited-Duration Insurance (STLDI) Plans
STLDI plans provide temporary coverage for a short period, typically up to 12 months. These plans are designed for individuals looking for short-term coverage or those waiting for employer insurance to kick in.
- Main Advantage: Lower premiums compared to other plan types, making them attractive to budget-conscious individuals.
- However, STLDI plans lack essential health benefits, such as mental health coverage, maternity care, and prescription medication.
- These plans often have exclusions, limitations, or waiting periods, which can leave you vulnerable to medical expenses.
Health Maintenance Organization (HMO) and Exclusive Provider Organization (EPO) Plans
HMO and EPO plans require you to see in-network providers for coverage. These plans can be a good choice for individuals who prefer a network of doctors and hospitals.
| Feature | HMO Plan | EPO Plan |
|---|---|---|
| Deductible | Higher deductibles (e.g., $1,000) | Lower deductibles (e.g., $500) |
| Network Restriction | Strict network restrictions | Less strict network restrictions |
| Cost-Sharing | Tends to have higher out-of-pocket costs | Tends to have lower out-of-pocket costs |
Health Reimbursement Arrangements (HRAs) and Flexible Spending Accounts (FSAs)
HRAs and FSAs allow you to set aside pre-tax dollars for medical expenses. These plans can help you save for deductibles, copays, and coinsurance.
- Main Advantage: Tax benefits, allowing you to save for medical expenses while reducing your taxable income.
- However, you’ll need to carefully budget and manage your HRA or FSA to avoid over-contributing and incurring penalties.
When making a decision, weigh the pros and cons of each plan, considering your age, health, and financial situation. If you’re experiencing health issues or are nearing retirement, it might be more beneficial to opt for a plan with lower deductibles and higher premiums. Conversely, if you’re a healthy individual under 30, a catastrophic plan or STLDI might be a more affordable choice. Ultimately, prioritize your financial security and access to quality healthcare services while choosing the best plan for your unique needs.
Closing Notes
So, what’s the bottom line? With Federal Blue Cross Blue Shield 2026 rates, it’s essential to be informed and proactive about your health. Don’t get left behind – stay ahead of the game and make the most out of your healthcare benefits.
Question & Answer Hub
What are the main factors affecting Federal Blue Cross Blue Shield 2026 rates?
The main factors include policy maker decisions, demographic changes, and healthcare trends.
How will Federal Blue Cross Blue Shield 2026 rates impact different age groups?
The rates will have varying impacts on different age groups, with some groups experiencing higher costs while others may see relief.
Are there any tax exemptions or subsidies available to help with Federal Blue Cross Blue Shield 2026 rates?
Certain groups may be eligible for tax exemptions or subsidies to help offset the costs of the new rates.