Cms medicare advantage star ratings 2026 released, the narrative unfolds in a compelling and distinctive manner, drawing readers into a story that promises to be both engaging and uniquely memorable.
The star rating system is crucial for Medicare Advantage beneficiaries as it significantly impacts their coverage and costs. For 2026, CMS has introduced updates to the rating criteria that beneficiaries need to be aware of.
Understanding the 2026 CMS Medicare Advantage Star Ratings and Their Impact on Beneficiaries
The Centers for Medicare & Medicaid Services (CMS) has released the 2026 Medicare Advantage Star Ratings, which evaluate the quality of Medicare Advantage (MA) plans offered by private insurers. These ratings can significantly impact beneficiaries’ choices of plans, as well as the costs and benefits associated with them.
The star rating system, which has been in place since 2009, assigns a grade from 1 to 5 stars to each MA plan based on its performance in various areas, such as quality of care, customer service, and extra benefits. The rating process involves collecting data from various sources, including claims data, surveys, and quality measures.
Updated Star Rating Criteria for 2026
Starting in 2026, CMS is introducing several updates to the star rating criteria, including:
Changes to Quality Measures
CMS is introducing new quality measures, such as the use of electronic health records, patient engagement, and care coordination. These measures are designed to promote better patient outcomes and more effective care management.
The updated star rating criteria will give beneficiaries a more comprehensive view of a plan’s quality and patient-centeredness.
New Category: Member Satisfaction with Provider Network
In 2026, CMS is adding a new category to the star rating system: member satisfaction with the provider network. This category will assess beneficiaries’ satisfaction with the plan’s network of healthcare providers, including physicians, hospitals, and other medical facilities.
Effects of Updated Star Ratings on Medicare Advantage Beneficiaries
The updated star ratings can have several effects on Medicare Advantage beneficiaries, including:
Changes to Benefits and Costs
Plans with lower star ratings may be more likely to reduce benefits or increase costs. Conversely, plans with higher star ratings may offer more comprehensive benefits or lower costs.
- Beneficiaries may see changes to their plan’s benefits, such as reduced coverage for certain services or medications.
- Beneficiaries may experience changes to their plan’s costs, such as increased premium rates or deductible amounts.
Changes to Provider Networks, Cms medicare advantage star ratings 2026 released
Plans with lower star ratings may be more likely to make changes to their network of healthcare providers, including removing high-cost or low-performing providers. This can impact beneficiaries’ access to care and their satisfaction with their provider network.
Using Star Ratings to Make Informed Decisions
Beneficiaries can use the star ratings to make informed decisions about their MA coverage by:
- Evaluating the plan’s overall star rating to determine its quality and performance.
- Reviewing the plan’s ratings in specific areas, such as quality of care, customer service, and extra benefits.
- Comparing the plan’s ratings to those of other MA plans in their area.
Beneficiaries should carefully review the star ratings and other plan characteristics before making a decision about their Medicare Advantage coverage.
Comparing 2026 Star Ratings to Previous Years
The 2026 star ratings show some significant changes compared to previous years, including:
Increases in Overall Star Ratings
On average, MA plans have seen an increase in their overall star ratings, with many plans achieving 4-star or higher ratings.
- For example, in 2025, the average overall star rating for MA plans was 3.8 stars. In 2026, the average overall star rating has increased to 4.2 stars.
Changes in Ratings by Category
There have been some notable changes in ratings by category, including:
- Quality of care: MA plans have seen an increase in their quality of care ratings, with many plans achieving 4-star or higher ratings.
- Customer service: MA plans have seen a slight decrease in their customer service ratings, with some plans experiencing issues with communication and claims processing.
Changes to Medicare Advantage Star Ratings in 2026: Cms Medicare Advantage Star Ratings 2026 Released
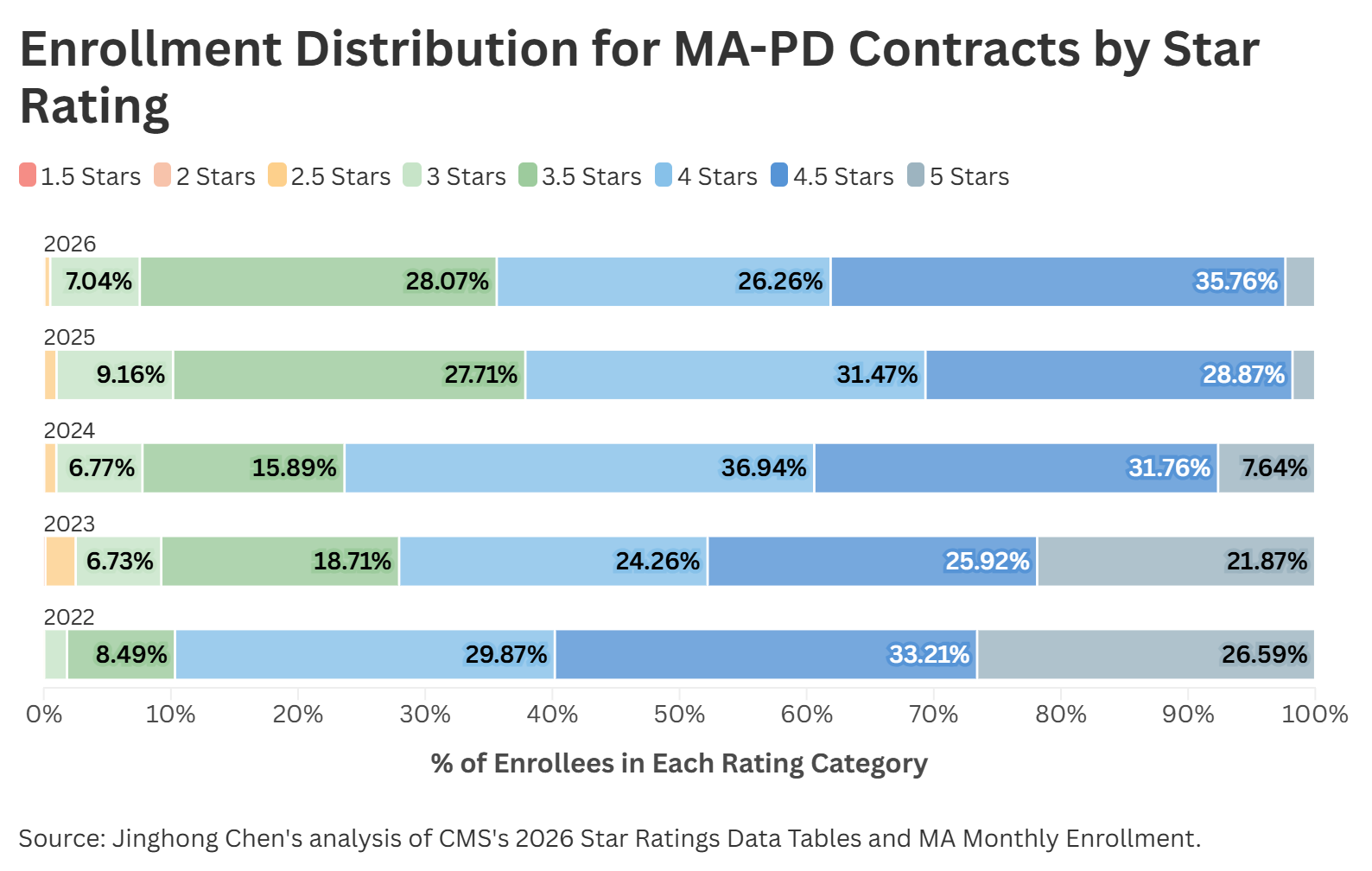
The Centers for Medicare and Medicaid Services (CMS) has announced the 2026 Medicare Advantage Star Ratings, introducing significant changes to the rating criteria. These updates aim to ensure that Medicare Advantage plans provide high-quality care to beneficiaries, while also promoting competition and innovation in the market. The changes will have a significant impact on Medicare Advantage plan providers, affecting their business operations, market share, and ultimately, the services they offer to beneficiaries.
Updated Rating Criteria for 2026
The updated rating criteria for 2026 introduce several key changes, including:
The introduction of a new measure for medication adherence, which will assess a plan’s performance in managing chronic conditions like diabetes, hypertension, and cholesterol.
An updated measure for healthcare effectiveness data and information set (HEDIS), which will focus on improved health outcomes for beneficiaries with complex conditions.
A revised measure for patient engagement, which will prioritize personalized care and patient-centered approaches.
Changes to the Rating Process
The CMS will apply the new rating criteria in the following ways:
For plans that meet the requirements, the new measures will replace the old measures, reflecting the importance of medication adherence, improved health outcomes, and patient engagement.
For plans that do not meet the requirements, they will be penalized based on their performance in the new measures.
The CMS will use a weighted average of the new measures to calculate the overall star rating.
Implications for Medicare Advantage Plan Providers
The changes to the rating criteria will have significant implications for Medicare Advantage plan providers:
Plan providers must adapt to the new measures and prioritize medication adherence, improved health outcomes, and patient engagement in their care delivery models.
Failure to meet the new requirements may result in reduced market share, revenue, and reputation.
Providers who excel in the new measures will experience increased market share, revenue, and reputation, as well as opportunities to innovate and improve their services.
| Year | Medication Adherence Measure | HEDIS Measure | Patient Engagement Measure |
|---|---|---|---|
| 2024 | Not included | Old HEDIS measure | Old patient engagement measure |
| 2025 | Optional measure | Updated HEDIS measure | Updated patient engagement measure |
| 2026 | Required measure | Revised HEDIS measure | Revised patient engagement measure |
Implementation Timeline
The CMS will implement the updated rating criteria as follows:
The new measures will be announced in the summer of 2026, with detailed instructions and guidance provided.
The CMS will begin evaluating plan performance using the new measures on a quarterly basis, with the first set of results released in the fall of 2026.
Plan providers will have one year to adapt to the new measures and improve their performance.
“The updated rating criteria will help ensure that Medicare Advantage plans prioritize high-quality care, patient engagement, and improved health outcomes for beneficiaries.” ~ CMS Director, Medicare Advantage Programs.
Resources and Support
The CMS will provide resources and support to help plan providers adapt to the updated rating criteria, including:
Training and webinars for plan administrators and providers.
Guidance documents and FAQs on the new measures and rating process.
Technical assistance for plans with limited resources or expertise.
Next Steps
Medicare Advantage plan providers should begin preparing for the updated rating criteria by:
Reviewing the new measures and rating process.
Assessing their current performance in the new measures.
Developing strategies to improve performance and adapt to the new measures.
Impact of 2026 CMS Medicare Advantage Star Ratings on Plan Provider Network and Benefits
The release of the 2026 CMS Medicare Advantage Star Ratings has significant implications for plan providers and beneficiaries alike. Top-performing plans will continue to attract new members, while lower-rated plans may struggle to retain existing ones. In response to these changes, plan providers are reassessing their provider networks, benefits, and cost structures to stay competitive.
Top-Performing Plans by Overall Star Rating
The following top-performing Medicare Advantage plans have achieved high overall star ratings, demonstrating exceptional quality and service delivery. These plans offer enhanced benefits and features that contribute to their high ratings.
- Humana Gold Plus’: 4.5/5 This plan stands out for its comprehensive network of 85,000 providers, including primary care physicians and specialists. It also offers a range of extra benefits, including meal delivery and transportation services.
- Aetna Medicare Value Plan: 4.5/5 This plan boasts a provider network of over 90,000 healthcare professionals. It also offers advanced telemedicine services, including virtual consultations with board-certified physicians.
- Anthem Choice: 4.5/5 This plan provides its members with access to over 120,000 providers nationwide. It also offers advanced personalized care programs, including coordinated care for chronic conditions.
To compete with top-performing plans, lower-rated plans are likely to reevaluate their provider networks, benefits, and cost structures. Some may choose to expand their networks or enhance existing benefits to improve their overall star ratings. Alternatively, they may opt to reduce costs or adjust their pricing models to appeal to price-conscious beneficiaries.
Benefit Comparison: Top-Performing Plans vs. Lower-Rated Plans
The benefits offered by top-performing plans differ significantly from those of lower-rated plans. While top-performing plans tend to provide more comprehensive networks, additional benefits, and advanced features, lower-rated plans may have limited provider networks and fewer extra benefits. This comparison highlights the importance of carefully evaluating plan benefits and ratings when making an informed decision about Medicare coverage.
| Benefit Category | Top-Performing Plans | Lower-Rated Plans |
|---|---|---|
| Provider Network | 85,000+ providers | 20,000+ providers |
| Additional Benefits | Meal delivery, transportation services | Limited or no additional benefits |
| Cost Structure | Competitive pricing | Higher premiums |
Plan providers closely tied to star ratings offer benefits that directly impact member satisfaction and quality of care. Changes to these benefits in 2026 reflect evolving member needs and preferences. Some key benefits most closely tied to star ratings include:
Benefits Most Closely Tied to Star Ratings
The following benefits are closely tied to star ratings and have undergone changes in 2026. Plan providers are adapting these benefits to better meet the needs of their members and enhance overall quality ratings.
- Telemedicine Services: Top-performing plans now offer advanced telemedicine services, including virtual consultations with board-certified physicians. These services have improved member convenience and access to quality care.
- Personalized Care Programs: Anthem Choice has expanded its personalized care programs, including coordinated care for chronic conditions. This approach has contributed to its high overall star rating.
- Meal Delivery and Transportation Services: Humana Gold Plus has incorporated meal delivery and transportation services, enhancing member convenience and support.
The Role of Technology in Enhancing Transparency and Understanding of the Medicare Advantage Star Ratings

In today’s digital age, technology plays a vital role in providing beneficiaries with accurate and comprehensive information about Medicare Advantage Star Ratings. Digital platforms and other technologies have significantly enhanced the accessibility and understanding of these ratings, empowering beneficiaries to make informed decisions about their healthcare.
Technology has enabled the development of user-friendly mobile apps, online tools, and data analytics platforms that help beneficiaries navigate the star ratings system. These tools provide real-time updates, allow users to compare different plans, and offer personalized recommendations based on their specific needs.
Enhancing Transparency with Digital Platforms
Digital platforms have revolutionized the way beneficiaries access and understand Medicare Advantage Star Ratings. These platforms offer a range of benefits, including:
– Real-time updates on star ratings and plan performance
– Comparative analysis of different plans and their benefits
– Personalized recommendations based on user-specific needs
– Easy access to plan details, including coverage, network, and premium costs
The Role of Data Analytics and Artificial Intelligence
Data analytics and artificial intelligence (AI) have the potential to significantly enhance the transparency and accountability of the star ratings system. These technologies can help identify areas of improvement, provide real-time feedback, and enable data-driven decision-making. AI-powered chatbots can also assist beneficiaries in understanding the star ratings system, answering frequently asked questions, and guiding them through the process of plan selection.
Key Digital Platforms and Technologies
The following are some of the key digital platforms and technologies that can help beneficiaries access and understand the 2026 star ratings:
- Medicare.gov: The official Medicare website provides a comprehensive overview of Medicare Advantage Star Ratings, including plan performance and ratings.
- Medicare Plan Finder: This tool allows beneficiaries to compare different Medicare Advantage plans and their benefits in real-time.
- Mobile Apps: Various mobile apps, such as Medicare Advisor and Medicare Navigator, provide personalized recommendations and real-time updates on plan performance.
- Data Analytics Platforms: Companies like Change Healthcare and Optum offer data analytics platforms that provide real-time insights and recommendations for Medicare Advantage plans.
- Artificial Intelligence-Powered Chatbots: AI-powered chatbots, such as those offered by Medicare and private companies, can assist beneficiaries in understanding the star ratings system and plan selection.
Final Thoughts

The release of the 2026 CMS Medicare Advantage star ratings brings about significant changes to the way beneficiaries navigate their Medicare coverage. It is essential to understand the implications and use the star ratings to make informed decisions about their Medicare plan.
FAQ Corner
What are the changes to the star rating system for 2026?
The changes to the star rating system for 2026 include updated rating criteria and a revised evaluation process. Beneficiaries can expect improved quality measures and enhanced transparency in the system.
How will the updated star ratings impact Medicare Advantage beneficiaries?
The updated star ratings will impact beneficiaries in terms of coverage, costs, and provider networks. Higher-rated plans may offer more benefits and better quality care, while lower-rated plans may experience changes to their provider networks or benefits.
Can beneficiaries use the star ratings to evaluate plans?
What role does technology play in the star ratings system?
Technology plays a significant role in the star ratings system, providing beneficiaries with easy access to plan information and quality data. Digital platforms and online tools can help beneficiaries navigate the system and make informed decisions about their Medicare coverage.