As ACA Maximum Out of Pocket 2026 takes center stage, this essential information helps readers navigate the complexities of health insurance, ensuring a clear understanding of the costs associated with healthcare services.
Understanding the ACA Maximum Out of Pocket (MOOP) costs is crucial for individuals and families seeking cost-effective health insurance plans. The MOOP limit, also known as the out-of-pocket maximum, is the maximum amount individuals must pay for healthcare expenses before their insurance plan kicks in to cover remaining costs. For 2026, this limit plays a significant role in determining healthcare expenses and subsidies for beneficiaries.
Understanding the ACA Maximum Out-of-Pocket (MOOP) Costs for 2026
Healthcare expenses can be a significant financial burden, and understanding the Maximum Out-of-Pocket (MOOP) costs is crucial for cost-effective planning. The MOOP cost is calculated by health insurance companies and sets a limit on the amount an individual or family has to pay for healthcare expenses in a year. This article will delve into the calculations of MOOP costs and its implications for beneficiaries.
The MOOP cost calculation involves various factors, including the premium cost, deductible, copayments, and coinsurance rates. According to the Affordable Care Act (ACA), health insurance companies must include an annual maximum out-of-pocket limit in their plans. This limit varies based on the plan type and metal level, with lower-cost plans (catastrophic plans) having a higher MOOP limit.
Components of MOOP Cost Calculation
The MOOP cost calculation is a complex process that involves several components. These components include:
- Premium Cost: The premium cost is the monthly amount an individual or family pays for health insurance coverage.
- Deductible: The deductible is the amount an individual or family must pay out-of-pocket before the insurance coverage kicks in.
- Copayments: Copayments are a fixed amount an individual pays for a specific healthcare service or doctor visit.
- Coinsurance Rates: Coinsurance rates are the percentage of healthcare expenses that an individual or family must pay after meeting the deductible.
The MOOP cost calculation starts with the premium cost, which is the monthly amount paid for health insurance coverage. The deductible is then added to the premium cost, followed by the copayments and coinsurance rates.
Examples of MOOP Cost Calculations, Aca maximum out of pocket 2026
Let’s consider an example to illustrate the MOOP cost calculation. Suppose an individual has a bronze plan with a premium cost of $300 per month, a deductible of $1,500, and copayments and coinsurance rates as follows:
- Copayments: $20 for doctor visits and $50 for prescription medications
- Coinsurance Rates: 30% for hospital stays and 20% for specialist visits
Using the above example, let’s calculate the MOOP cost for a year.
MOP = (12 * premium) + deductible + (sum of copays) + (sum of coinsurance)
MOP = (12 * 300) + 1500 + (12 * 20) + (12 * 50) + (sum of coinsurance)
MOP = 3600 + 1500 + 240 + 600 + (sum of coinsurance)
Assuming the individual has a hospital stay with a bill of $10,000 and a specialist visit with a bill of $5,000, the sum of coinsurance would be:
(30% of 10000) + (20% of 5000) = 3000 + 1000 = 4000
Now, let’s calculate the total MOOP cost for the year:
MOP = 3600 + 1500 + 240 + 600 + 4000 = 9440
In conclusion, the MOOP cost calculation is a complex process that involves several components. Understanding these calculations is crucial for cost-effective planning and making informed decisions about healthcare expenses.
Current MOOP Limits for the ACA Marketplace and How They Affect Subsidies

The maximum out-of-pocket (MOOP) limits for the Affordable Care Act (ACA) marketplace have been increasing to accommodate rising healthcare costs. Understanding these limits is crucial for individuals and families seeking affordable health insurance plans. By examining the MOOP limits for the ACA marketplace, Medicaid, and other healthcare programs, we can better grasp how these differences affect subsidies and healthcare financing.
Comparison of MOOP Limits
MOOP limits serve as the maximum amount an individual or family must pay for healthcare expenses before subsidies kick in. Here’s a comparison of MOOP limits for the ACA marketplace, Medicaid, and other healthcare programs:
| Program | MOOP Limit (2026) |
| — | — |
| ACA Marketplace (Silver Plan) | $8,900 Individual, $22,000 Family |
| ACA Marketplace (Gold Plan) | $7,400 Individual, $18,700 Family |
| Medicaid | No MOOP (complimentary benefits) |
| Employer-Sponsored Insurance | Varies, often $7,000-$10,000 |
| Medicare Advantage | $7,550 Individual, $15,300 Couple |
MOOP Limits and Subsidies
MOOP limits are essential in determining health insurance plan pricing and accessibility, particularly for those with pre-existing conditions. When MOOP limits are higher, subsidies become more significant, making health insurance more affordable. Here’s an example of how MOOP limits impact subsidies:
* For an individual with an annual income of $25,000, the premium tax credit (subsidy) would cover the difference between 9.5% and 400% of their income. With an MOOP limit of $8,900, they would receive a larger subsidy, making the premium more affordable.
* In contrast, if the MOOP limit decreased to $5,000, the subsidy might be reduced, making the premium less affordable for this individual.
MOOP Limits and Healthcare Financing
MOOP limits also affect healthcare financing by influencing an individual’s or family’s ability to access care. When MOOP limits are higher, individuals and families are more likely to exhaust their savings, take on medical debt, or experience financial hardship. This can lead to:
* Increased financial burden on individuals and families
* Rationing of medical care due to cost constraints
* Decreased access to preventive care and screenings
* Negative impacts on health outcomes and overall well-being
Implications for Those with Pre-Existing Conditions
MOOP limits have a disproportionate impact on individuals with pre-existing conditions. Those with chronic conditions or ongoing treatments often face higher healthcare costs, which can quickly exceed MOOP limits.
* Without adequate subsidies, individuals with pre-existing conditions may be pushed into higher-cost plans or face steep out-of-pocket costs.
* This can lead to reduced access to necessary care, compromising health outcomes and overall well-being.
* Increased MOOP limits can also exacerbate healthcare disparities, as those with pre-existing conditions are already disproportionately affected by healthcare costs.
By understanding the current MOOP limits for the ACA marketplace and their impact on subsidies, we can better appreciate the importance of affordable healthcare financing for individuals and families. This knowledge can inform policy discussions and advocacy efforts aimed at reducing healthcare costs and improving access to affordable care.
MOOP Costs for Different Healthcare Services and Treatment Options
Understanding the intricacies of Maximum Out-of-Pocket (MOOP) costs can seem daunting, but it’s essential for consumers to grasp the nuances to make informed decisions about their healthcare expenses. MOOP costs refer to the maximum amount an individual or family must pay out-of-pocket for healthcare services, including doctor visits, hospital stays, prescription medications, and other expenses in a given year.
Doctor Visits and Medical Services
The MOOP costs for doctor visits and medical services can vary significantly depending on the type of visit, location, and provider. For example, a routine doctor visit might cost around $50-$100, whereas a specialist visit could range from $100 to $200 or more. In addition, services like lab tests, imaging studies, and other diagnostic tests can add up quickly, with costs ranging from $100 to $1,000 or more per test.
- Skin exams: $50-$200
- Vaccinations: $20-$100
- Basic lab tests (blood work): $50-$300
- Advanced lab tests (imaging): $100-$1,500
Prescription Medications and Specialty Treatments
MOOP costs for prescription medications can also be substantial, depending on the type of medication, dosage, and frequency of use. Specialty treatments like chemotherapy, infusion therapies, or injectables can be particularly costly, with prices ranging from $50 to $20,000 or more per treatment cycle.
- Cortisol replacement therapy: $50-$100/month
- Anti-inflammatory medications: $20-$50/month
- Cancer treatments (chemotherapy): $5,000-$20,000/mo cycle
- Hormone replacement therapy: $50-$100/month
Hospital Stays and Surgery
MOOP costs for hospital stays and surgeries can be exorbitant, with prices ranging from $10,000 to $100,000 or more per case. The cost of hospital stays can be further complicated by factors like length of stay, type of surgery, and level of care required.
| Procedure | Cost Range |
|---|---|
| Appendectomy | $10,000-$50,000 |
| Cholecystectomy | $20,000-$80,000 |
| Joint replacement | $30,000-$100,000 |
Mitigating Strategies for High MOOP Costs and Unaffordable Healthcare: Aca Maximum Out Of Pocket 2026
When it comes to dealing with the high costs associated with Affordable Care Act (ACA) maximum out-of-pocket (MOOP) expenses, consumers are left scrambling for ways to stay afloat. It’s time to break free from the cycle of high medical bills and explore some savvy strategies to mitigate the financial strain.
Shopping for Affordable Plans
Finding the most cost-effective health insurance plan can be a daunting task, especially when sifting through various options in the marketplace. However, savvy shoppers can save a significant amount by taking the following steps:
- Compare plan networks and ensure that your favorite healthcare providers are included, minimizing the need for costly out-of-network claims.
- Look for plans with lower deductible options, which may come at the expense of higher monthly premiums.
- Consider plans with wellness programs or incentives for staying healthy, which can offset overall costs.
- Shop around during the open enrollment period or during special enrollment periods triggered by life events, such as job changes or marriage.
By taking a meticulous approach to plan comparison, consumers can make informed decisions that help them navigate the complex world of MOOP costs.
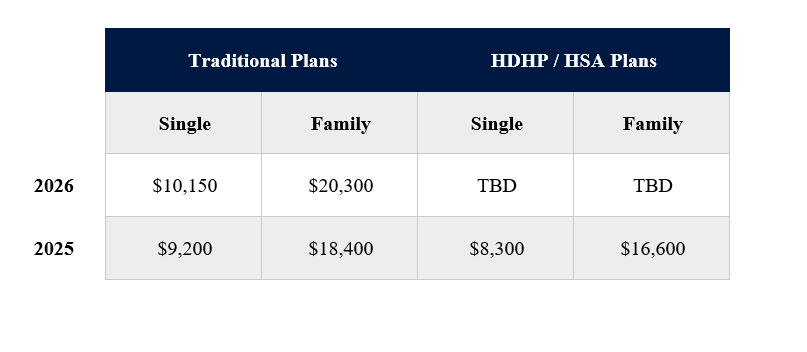
Utilizing Health Savings Accounts (HSAs)
A Health Savings Account (HSA) is a triple-tax-advantaged savings account that allows you to set aside funds for medical expenses, all while enjoying tax benefits. This clever tool can be leveraged to mitigate the financial burden of MOOP costs in several ways:
- Contribution limits for HSAs increase annually, making them an attractive option for those looking to save for future medical expenses. For example, in 2026, the individual coverage HSA limit is $3,600, while family coverage has a limit of $7,200.
- Unused HSA funds can be carried forward indefinitely, providing a secure nest egg for future medical expenses.
- HSA funds can be invested, allowing account holders to grow their savings over time, further reducing their MOOP burden.
- HSAs are often used in conjunction with high-deductible health plans (HDHPs), which can be paired with tax-deductible premiums and lower premiums, helping to reduce MOOP costs.
By harnessing the power of HSAs, consumers can proactively address their MOOP concerns, build a safety net, and make more informed healthcare decisions.
Employer-Sponsored Health Insurance
For large groups and small businesses, employer-sponsored health insurance is often the go-to solution for mitigating MOOP costs. These plans come with numerous benefits, including:
- Negotiated rates with healthcare providers, reducing the overall cost of care.
- Tax benefits for both employers and employees, as premiums are often tax-deductible and employee contributions are pre-tax.
- Comprehensive network options, providing access to a wide range of healthcare services and specialists.
- Wellness programs and employee incentives, promoting healthy behavior and reducing MOOP costs.
Employer-sponsored health insurance offers a reliable way for large groups and small businesses to manage MOOP costs, ensuring that their employees have access to quality care while minimizing financial burdens.
The Interplay between MOOP Costs and Other Health Insurance Policies
In the complex world of health insurance, numerous factors converge to shape the financial burdens on patients. While the Affordable Care Act (ACA) established maximum out-of-pocket (MOOP) costs, other health insurance policies like Medicare, Medicaid, and private employer-sponsored plans also have distinct cost-sharing parameters. Understanding the intersection of MOOP costs and these other policies is crucial for navigating the healthcare landscape.
The MOOP costs established by the ACA serve as a safeguard against catastrophic expenses, capping the total out-of-pocket expenses a patient can face in a given year. However, when paired with other health insurance policies, the MOOP costs can be influenced in various ways.
MOOP Costs and Medicare
Medicare, a federal health insurance program for seniors and individuals with disabilities, operates under its own MOOP cost structure. The Medicare Part D Prescription Drug Benefit program has a separate MOOP cost, known as the true out-of-pocket (TrOOP) limit. This limit allows beneficiaries to avoid the Medicare gap, also known as the coverage gap, where they would be responsible for a portion of prescription drug costs.
Medicare MOOP Costs Comparison
| Medicare Program | MOOP Costs |
| — | — |
| Part D Prescription Drug Benefit | TrOOP Limit: $2,850 |
| Medicare Advantage (MA) Plans | MOOP Costs Vary by Plan |
When Medicare is combined with a Marketplace plan or another employer-sponsored plan, the MOOP costs from each plan are not automatically combined. However, the Medicare beneficiary still needs to meet the MOOP costs of the Medicare Part D plan. It is essential to understand the MOOP costs of each plan to avoid surprise medical bills.
MOOP Costs and Medicaid
Medicaid, a joint federal-state program, provides health insurance coverage to low-income individuals and families. The MOOP costs for Medicaid vary by state, as each state sets its own cost-sharing parameters. Generally, Medicaid has lower MOOP costs compared to private insurance plans, with some plans offering minimal or no cost-sharing.
Medicaid MOOP Costs Comparison
| Medicaid Program | MOOP Costs |
| — | — |
| Standard Medicaid Plan | Lower MOOP Costs, Varying by State |
| Medicaid Managed Care Plans | MOOP Costs Vary by Plan |
When Medicaid beneficiaries have a private insurance plan or a Marketplace plan, they may still meet the MOOP costs of that plan, even if they have Medicaid coverage. Therefore, it is crucial to understand the MOOP costs of both plans to avoid any potential financial burdens.
MOOP Costs and Private Employer-Sponsored Plans
Private employer-sponsored plans, also known as group health plans, have their own MOOP costs and cost-sharing parameters. These plans can have higher MOOP costs compared to Marketplace plans, but they may offer more comprehensive coverage.
Private Employer-Sponsored Plans MOOP Costs Comparison
| Private Employer-Sponsored Plan | MOOP Costs |
| — | — |
| Group Health Plan | Higher MOOP Costs, Varying by Plan |
When an employee has both a private employer-sponsored plan and a Marketplace plan, the MOOP costs of each plan are not necessarily combined. The employee may still need to meet the MOOP costs of each plan, which can lead to surprise medical bills.
In conclusion, understanding the interplay between MOOP costs and other health insurance policies is essential for navigating the complex healthcare landscape. By being aware of the MOOP costs and cost-sharing parameters of each plan, individuals and families can make informed decisions and avoid surprise medical bills.
Final Summary
With the ACA Maximum Out of Pocket 2026, it’s essential for beneficiaries to stay informed about MOOP costs, plan pricing, and accessibility. By understanding the intricacies of MOOP costs, individuals can make informed decisions about their healthcare, choose cost-effective plans, and access necessary treatment without breaking the bank.
Answers to Common Questions
What is the maximum MOOP limit for 2026 under the ACA?
The maximum MOOP limit for 2026 under the Affordable Care Act (ACA) is $8,800 for individuals and $17,400 for families.
How does the MOOP affect health insurance plan pricing?
The MOOP limit affects health insurance plan pricing as it determines the maximum amount individuals must pay for healthcare expenses. This, in turn, influences plan pricing and accessibility for beneficiaries.
What are some strategies to mitigate high MOOP costs?
Several strategies can help mitigate high MOOP costs, including shopping for affordable health insurance plans, using Health Savings Accounts (HSAs), and negotiating medical bills.
Can I access tax benefits with employer-sponsored health insurance?
Yes, employer-sponsored health insurance plans often offer tax benefits, such as pre-tax contributions to HSA or medical reimbursement plans.