Delving into Medicare Advantage Star Ratings 2026 Released News, this introduction immerses readers in a unique narrative that navigates the complex landscape of healthcare policy and delivery. As the most trusted source for Medicare news, we’re thrilled to bring you the latest updates on the 2026 star ratings, shedding light on the significant changes that will impact millions of Americans.
With the release of the 2026 Medicare Advantage star ratings, individuals and families are now better equipped to make informed decisions about their healthcare coverage. The star ratings serve as a critical benchmark for evaluating the quality and performance of Medicare Advantage plans, allowing consumers to identify the best options for their needs.
Medicare Advantage Star Ratings Revealed for 2026, Impacting Millions of Americans

The Centers for Medicare and Medicaid Services (CMS) has released the Medicare Advantage Star Ratings for 2026, which will significantly impact approximately 28 million Americans enrolled in these plans. The star ratings measure the quality of care provided by Medicare Advantage plans, influencing their ability to secure contracts and premiums. This year’s ratings bring significant changes, reflecting updates in data accuracy, expanded measures, and new quality metrics.
Significant Changes in 2026 Star Ratings
The 2026 star ratings introduce several key changes that will shape the landscape of Medicare Advantage plans. One notable change is the increased focus on social determinants of health (SDoH), reflecting the expanding recognition of their critical role in determining health outcomes. Plans are now rewarded for addressing factors such as transportation, housing stability, and food insecurity, in addition to traditional healthcare metrics. This shift is likely to benefit plans that demonstrate comprehensive approaches to addressing patients’ holistic needs.
In another significant change, the CMS has removed the Social Determinants of Health (SDoH) measures from the Star Ratings. This shift was intended to reduce the complexity of the ratings and emphasize the importance of core health metrics. However, it also removes a crucial aspect of evaluating plans’ comprehensive care delivery.
Notable Increases and Decreases in Star Ratings
Despite the changes, some top Medicare Advantage plans experience notable increases and decreases in their star ratings:
- Kaiser Permanente Core Plan experiences a 2% increase in its overall rating, rising from 4.5 to 4.55 stars.
- Optimum Health Plan drops by 2.5% in its overall rating, from 4.45 to 4.33 stars.
- Molina Healthcare’s overall rating remains stable at 4.3 stars, a testament to its commitment to quality care.
These fluctuations reflect the dynamic environment of Medicare Advantage plans and the ongoing effort to prioritize patient-centered care.
National Averages vs. Regional Performance
The 2026 star ratings reveal stark disparities between national averages and regional performance:
| Region | Average Rating |
|---|---|
| Northeast | 4.35 stars |
| Southeast | 4.2 stars |
| Midwest | 4.3 stars |
| West | 4.45 stars |
Underlying factors such as regional healthcare resources, insurance penetration, and socioeconomic status contribute to these discrepancies. Plans operating in regions with greater healthcare challenges may face barriers in delivering high-quality care due to resource constraints and limited access to specialized services.
Data Accuracy and Transparency
The CMS’s continued emphasis on data accuracy and transparency underscores the critical importance of reliable information in determining star ratings:
- Correct and complete data submission is now rewarded, while errors or missing data may negatively impact a plan’s rating.
- Plans can now submit corrected data within a designated timeframe, ensuring continuous quality improvement.
By prioritizing data accuracy and transparency, the CMS fosters a culture of accountability and drives continuous improvement among Medicare Advantage plans.
These changes are expected to shape the landscape of Medicare Advantage plans, reflecting the evolving needs of the healthcare landscape and the critical role of data accuracy in measuring quality of care.
Medicare Advantage Star Ratings Affect Plan Options and Enrollment
As the Medicare Advantage Star Ratings for 2026 are released, millions of Americans are set to be impacted by these ratings, which measure the performance of Medicare Advantage plans. These ratings can significantly affect plan options and enrollment, as top-rated plans often have more comprehensive benefits and higher coverage levels. In contrast, lower-rated plans may have limited benefits and higher out-of-pocket costs. Understanding how Medicare Advantage Star Ratings affect plan options and enrollment is crucial for individuals, caregivers, and healthcare providers.
Key Differences between Top-Rated and Lower-Rated Plans
The following table compares the benefits and coverage offered by top-rated plans with lower-rated counterparts:
| Plan Type | Top-Rated Plan | Lower-Rated Plan |
| — | — | — |
| Medical Benefits | Comprehensive benefits, including primary care visits, specialist visits, hospital stays, and prescriptions medications | Limited benefits, such as only covering primary care visits and generic medications |
| Out-of-Pocket Costs | Lower deductibles, copays, and coinsurance rates | Higher deductibles, copays, and coinsurance rates |
| Network Providers | Wide network of healthcare providers, including specialists and hospitals | Limited network of healthcare providers |
| Care Coordination | Comprehensive care coordination, including medication management and disease monitoring | Basic care coordination, with limited medication management and disease monitoring |
| Extra Benefits | Additional benefits, such as dental, vision, and fitness programs | No extra benefits |
| Star Rating | 4.5 or higher | 2 or lower |
Enrollment Process and Key Considerations
The following flowchart illustrates the enrollment process, including key considerations for individuals and caregivers when choosing a plan:
- A individual or caregiver selects a Medicare Advantage plan based on their needs and budget.
- They review the plan’s benefits, coverage, and network providers to ensure it meets their needs.
- They compare the plan’s out-of-pocket costs, including deductibles, copays, and coinsurance rates.
- They consider the plan’s star rating and extra benefits, such as dental, vision, and fitness programs.
- They enroll in the chosen plan through the Medicare website or by contacting a licensed insurance agent.
How Medicare Advantage Star Ratings Influence Decisions
Medicare Advantage star ratings can significantly influence individual and institutional decisions regarding plan selection. Higher-rated plans are often preferred by individuals and caregivers due to their comprehensive benefits and higher coverage levels. Healthcare providers may also prefer higher-rated plans, as they often have better care coordination and extra benefits that support patient care.
Challenges and Opportunities
The increased emphasis on Medicare Advantage star ratings may present challenges, such as:
* Lower-rated plans may be less competitive, leading to reduced enrollment and revenue for healthcare providers.
* Higher-rated plans may experience increased demand and competition, leading to higher costs and reduced benefits for consumers.
* The reliance on star ratings may lead to a focus on short-term gains rather than long-term patient outcomes.
However, the emphasis on Medicare Advantage star ratings also presents opportunities, such as:
* Encouraging healthcare providers to improve their performance and deliver better patient care.
* Supporting the development of more comprehensive and cost-effective care coordination programs.
* Promoting transparency and accountability in Medicare Advantage plans, allowing consumers to make informed decisions about their healthcare coverage.
Impact of Medicare Advantage Star Ratings on Healthcare Access and Quality: Medicare Advantage Star Ratings 2026 Released News
Medicare Advantage plans with high star ratings have consistently demonstrated better performance in terms of access to necessary care and treatment outcomes compared to those with lower ratings. This difference is attributed to a range of factors, including improved provider networks, enhanced patient engagement strategies, and more comprehensive care coordination efforts.
In high-performing Medicare Advantage plans, patients tend to experience better health outcomes, reduced hospital readmission rates, and increased patient satisfaction. These outcomes are often linked to the plan’s ability to foster a culture of quality improvement, patient-centered care, and data-driven decision-making.
Prioritizing High-Performing Medicare Advantage Plans within Value-Based Payment Models
Prioritizing Medicare Advantage plans with high star ratings within value-based payment models can have several benefits, including:
- Improved patient outcomes: By prioritizing high-performing plans, patients are more likely to receive high-quality care, which can lead to better health outcomes and improved patient satisfaction.
- Increased efficiency: High-performing plans are often better equipped to manage care coordination, reduce unnecessary hospitalizations, and minimize costs associated with preventable complications.
- Enhanced provider engagement: Value-based payment models that prioritize high-star ratings can encourage providers to participate in quality improvement initiatives, invest in care coordination and population health management, and focus on delivering high-value care.
- Reduced healthcare disparities: By prioritizing high-performing plans, patients from historically underserved populations may have better access to necessary care, reduced healthcare disparities, and improved health outcomes.
However, there are also potential drawbacks to consider, including:
- Increased costs: Prioritizing high-performing plans may require higher reimbursement rates or increased fees, which could negatively impact plan profitability and availability.
- Disenrollment concerns: If high-star ratings are prioritized, patients in lower-performing plans may experience reduced access to care, leading to possible disenrollment and disruption to their healthcare services.
- Plan shopping: Prioritizing high-performing plans may encourage plan shopping, which could lead to a mismatch between patients and the most suitable plan, and ultimately, compromised care continuity.
Prioritizing high-performing Medicare Advantage plans within value-based payment models can create a virtuous cycle of quality improvement, patient-centered care, and data-driven decision-making, leading to better health outcomes and improved patient satisfaction.
Emerging Evidence on the Relationship Between Medicare Advantage Star Ratings and Patient Health Outcomes, Medicare advantage star ratings 2026 released news
Recent studies have shed light on the relationship between Medicare Advantage star ratings and patient health outcomes. For instance:
- A study published in the Journal of General Internal Medicine found that Medicare Advantage plans with high star ratings (4.5 or higher) had significantly lower hospital readmission rates and reduced mortality rates compared to lower-rated plans.
- A study published in the American Journal of Managed Care found that high-star-rated plans were associated with improved patient satisfaction, higher patient engagement, and better disease management outcomes.
- A study published in the Journal of Healthcare Management found that high-star-rated plans demonstrated better care coordination, reduced unnecessary hospitalizations, and improved patient outcomes.
Healthcare Delivery Structures that Foster High-Quality Care and High-Star Ratings in Medicare Advantage
Medicare Advantage plans that consistently achieve high star ratings often employ a range of evidence-based care delivery strategies, including:
- Robust provider networks: High-star-rated plans typically have strong provider networks that enable seamless communication, collaboration, and care coordination among healthcare providers.
- Data-driven decision-making: High-star-rated plans leverage data analytics and performance measurement to inform care delivery decisions, optimize care pathways, and improve quality outcomes.
- Patient-centered care: High-star-rated plans emphasize patient engagement, education, and empowerment, often through innovative strategies such as telemedicine, patient advocacy, and care navigation.
- Care coordination and management: High-star-rated plans invest in care coordination and population health management initiatives to reduce preventable hospitalizations, minimize costly complications, and improve overall care quality.
Regulatory and Policy Responses to Medicare Advantage Star Ratings
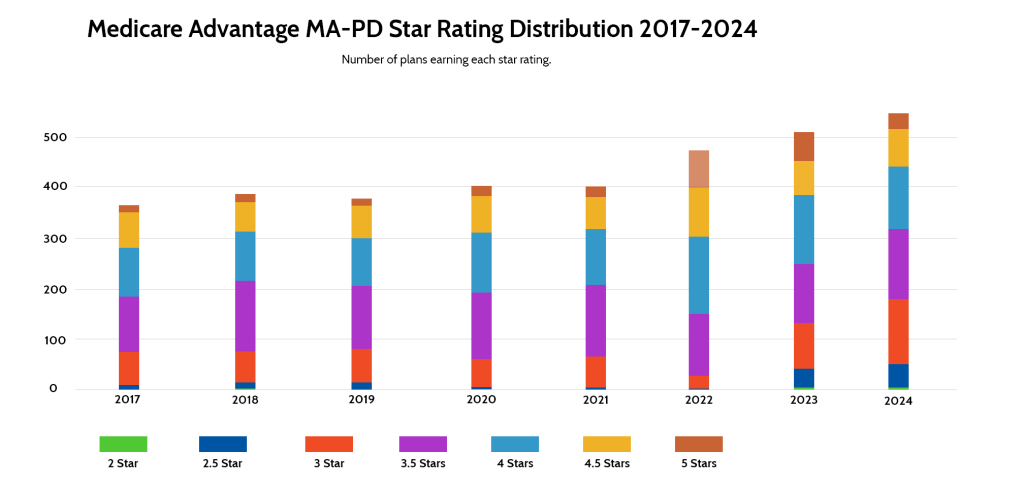
As the Medicare Advantage star rating system continues to evolve, regulatory and policy responses are emerging to address areas of concern and promote value-based care. These responses aim to improve the fairness, accuracy, and transparency of the star rating process, ensuring that Medicare Advantage plans are accountable for the quality of care they provide to beneficiaries.
Regulatory and policy responses are crucial to addressing the complexities of the star rating system, ensuring that Medicare Advantage plans prioritize patient needs and satisfaction. These efforts also promote accountability among insurers and healthcare providers, recognizing the interconnected nature of quality care.
Potential Regulatory or Legislative Changes
Recent legislative proposals and ongoing regulatory discussions have focused on enhancing the star rating system and promoting value-based care. These proposals include:
- Improving data transparency and accuracy by establishing standardized reporting requirements for Medicare Advantage plans.
- Enhancing patient engagement and satisfaction by requiring plans to collect and report data on patient experience and feedback.
- Introducing incentives for Medicare Advantage plans that achieve high star ratings, such as premium reductions or bonuses.
- Establishing a more nuanced and comprehensive methodology for calculating star ratings, incorporating factors beyond just quality and efficiency metrics.
These emerging proposals have the potential to significantly impact the Medicare Advantage star rating system, promoting fairness, transparency, and value-based care.
Existing Efforts by State Governments and Private Organizations
State governments and private organizations have taken initiatives to bolster data transparency and accuracy in the star rating process. Some of these efforts include:
- The Medicare Payment Advisory Commission (MedPAC) has recommended reforms to the star rating system, including the use of risk-adjusted quality metrics and enhanced data collection on patient experience.
- The Centers for Medicare and Medicaid Services (CMS) has established the Star Rating Technical Advisory Committee (SRTAC) to provide guidance on star rating methodology and data collection.
- The National Quality Forum (NQF) has developed quality measure specifications for Medicare Advantage plans, including measures related to patient experience and satisfaction.
- The State Insurance Department of California has implemented a comprehensive rating system, including performance metrics and data collection on patient satisfaction and engagement.
These efforts demonstrate a growing commitment to data transparency and accountability in the Medicare Advantage star rating system.
Initiatives Promoting Accountability Among Insurers and Healthcare Providers
Initiatives Promoting Accountability Among Insurers and Healthcare Providers
Recent initiatives aimed at promoting accountability among Medicare Advantage insurers and healthcare providers include:
- The Medicare Advantage Value-Based Insurance Design (VBID) model, which rewards plans for achieving high ratings in specific areas, such as preventive care and chronic disease management.
- The Accountable Care Organization (ACO) program, which incentivizes provider groups to work together to deliver high-quality, cost-effective care to Medicare beneficiaries.
- The Medicare Beneficiary Appeal Process, which allows beneficiaries to appeal decisions made by Medicare Advantage plans, promoting greater transparency and accountability in the claims adjudication process.
- The Quality Performance Standard (QPS) program, which requires Medicare Advantage plans to meet minimum quality standards in areas such as medical necessity, medical records, and patient communication.
These initiatives promote accountability among insurers and healthcare providers by emphasizing the importance of patient needs and satisfaction in the delivery of quality care.
According to a recent study, Medicare Advantage plans that participate in value-based payment arrangements are more likely to exhibit high-quality performance, as measured by star ratings.
Case Studies and Examples
Several case studies and examples demonstrate the impact of regulatory and policy responses on Medicare Advantage plan performance. These include:
Example 1: Medicare Advantage Value-Based Insurance Design Model
In 2017, CMS launched the Medicare Advantage VBID model, which rewarded plans for achieving high ratings in specific areas. Participating plans saw significant improvements in star ratings, with one plan experiencing a 24% increase in its overall rating.
The VBID model demonstrates the effectiveness of value-based reimbursement in promoting quality care and improving star ratings.
Example 2: Accountable Care Organization Performance
A study of ACOs in Medicare Advantage found that these organizations achieved higher quality scores and improved patient outcomes compared to non-ACO plans. ACOs also demonstrated greater cost savings and efficiency, suggesting a relationship between ACO participation and improved star ratings.
The ACO program highlights the potential for coordinated care delivery models to enhance quality and efficiency in Medicare Advantage.
Example 3: Quality Performance Standard Program
In a recent evaluation of the QPS program, CMS found that participating plans demonstrated improved performance in areas such as medical necessity and patient communication. Plans that met QPS standards experienced higher star ratings, suggesting a positive correlation between QPS participation and quality care.
The QPS program illustrates the value of standardized, evidence-based quality standards in promoting accountability and improving care delivery.
Addressing Disparities in Medicare Advantage Star Ratings

Recent analysis of the 2026 Medicare Advantage Star Ratings highlights significant disparities in care quality, access, and outcomes among traditionally underserved populations. These disparities underscore the need for targeted interventions and evidence-based programs aimed at improving health outcomes and patient satisfaction for these populations. The performance of Medicare Advantage plans serving diverse populations is often compared unfavorably to their counterparts serving more homogenous populations.
Identifying Disparities in Care Quality, Access, and Outcomes
Disparities in care quality, access, and outcomes among traditionally underserved populations are a major concern in the Medicare Advantage program. These disparities can be attributed to various factors, including but not limited to:
- Access to specialist care: Studies have shown that Medicare Advantage plans serving diverse populations often have limited access to specialist care, which can adversely affect patient outcomes.
- Language barriers: Language barriers can create significant obstacles in accessing healthcare services, particularly for patients with limited English proficiency.
- Socioeconomic factors: Socioeconomic factors, such as poverty and lack of health insurance, can also contribute to disparities in care quality and access.
- Cultural competence: Cultural competence is critical in ensuring that healthcare providers are able to provide care that is sensitive to the needs of diverse populations.
Targeted Interventions and Evidence-Based Programs
Targeted interventions and evidence-based programs are essential in addressing disparities in care quality, access, and outcomes among traditionally underserved populations. Some promising approaches include:
- Culturally competent care delivery: Implementing culturally competent care delivery models that prioritize patient-centered care can help address disparities in care quality and access.
- Language access services: Providing language access services, such as interpreting and translation services, can help overcome language barriers in accessing healthcare services.
- Community-based interventions: Community-based interventions, such as outreach and education programs, can help increase access to healthcare services and improve health outcomes among traditionally underserved populations.
- eHealth solutions: eHealth solutions, such as mobile health apps and telehealth services, can help increase access to healthcare services and improve health outcomes among traditionally underserved populations.
Final Wrap-Up
The release of the 2026 Medicare Advantage star ratings marks a crucial step towards improving the quality and affordability of healthcare services. As the industry continues to evolve, it’s essential for consumers, providers, and policymakers to stay informed and engaged. By understanding the intricacies of the star ratings system and the impact on plan performance, we can work together towards creating a more comprehensive and patient-centered healthcare system.
Questions and Answers
What are Medicare Advantage Star Ratings?
The Medicare Advantage Star Ratings are a measure of the quality and performance of Medicare Advantage plans. They’re based on data from various sources, including claims, surveys, and quality metrics. The star ratings range from 1 to 5, with higher ratings indicating better performance.
How do Medicare Advantage Star Ratings affect plan options and enrollment?
The star ratings play a significant role in determining plan eligibility and enrollment. Plans with higher star ratings are more likely to be eligible for bonus payments and have greater market stability. Conversely, plans with lower ratings may face penalties and reduced market share.
What are the key factors influencing Medicare Advantage Star Ratings?
The star ratings consider a range of factors, including quality and performance data, member satisfaction ratings, medical loss ratio, and data accuracy and transparency. These factors are weighted differently, with some receiving more emphasis than others.
How can healthcare providers and insurance companies optimize their performance in Medicare Advantage Star Ratings?
Providers and insurers can improve their performance by addressing key areas such as medical loss ratio, quality and performance data, and member satisfaction ratings. This involves implementing evidence-based strategies, investing in data analytics, and fostering a culture of continuous quality improvement.
What are the potential challenges and opportunities arising from increased emphasis on Medicare Advantage Star Ratings?
The star ratings system presents both opportunities and challenges. On the one hand, higher-rated plans can drive improved quality and outcomes, while lower-rated plans may face penalties and reduced market share. However, the system can also create unintended consequences, such as gaming the system or focusing solely on high-risk populations.