With 2026 bcbs medicare advantage plans at the forefront, this comprehensive guide aims to provide an in-depth understanding of the historical context, evolution, and significance of these plans to beneficiaries.
From eligibility requirements and enrollment processes to covered benefits, prescription drug coverage, and plan networks, this article will walk you through the intricacies of 2026 bcbs medicare advantage plans, empowering you with the knowledge to make informed decisions about your healthcare.
Understanding 2026 BCBS Medicare Advantage Plans and Their Significance
The Blue Cross Blue Shield (BCBS) Medicare Advantage Plans have been a vital part of the healthcare system in the United States for decades. The implementation of Medicare Advantage plans dates back to 1982, initially designed to provide an alternative to traditional fee-for-service Medicare. Over the years, these plans have undergone significant transformations, adapting to changes in the healthcare landscape and the needs of beneficiaries.
Historical Context of BCBS Medicare Advantage Plans
The Medicare program was enacted in 1965, providing health insurance coverage to individuals 65 years and older, as well as certain younger people with disabilities. Initially, Medicare covered hospital and medical services, but there was a need for a more comprehensive and cost-effective option. In response, Medicare Advantage plans were introduced as a part of the Omnibus Budget Reconciliation Act of 1982.
Medicare Advantage plans aimed to offer a fixed amount of money to the plan each month for each Medicare beneficiary. This approach, known as a capitated payment system, incentivized health plans to provide more efficient care, reduce hospitalizations, and increase preventive services. Over the years, Medicare Advantage plans have evolved to include various features, such as HMOs (Health Maintenance Organizations), PPOs (Preferred Provider Organizations), SNPs (Special Needs Plans), and MSAs (Medicare Savings Accounts).
Evolution of Medicare Advantage Plans
The Medicare Modernization Act of 2003 introduced several key changes to Medicare Advantage plans. This legislation created the Medicare Prescription Drug, Improvement, and Modernization Act, which allowed Medicare Advantage plans to offer prescription drug coverage, known as Medicare Part D. This expansion marked a significant shift in the scope of Medicare Advantage plans, enabling them to provide a more comprehensive package of benefits.
In 2010, the Patient Protection and Affordable Care Act (ACA) added further changes to Medicare Advantage plans. The ACA introduced accountable care organizations (ACOs) and required Medicare Advantage plans to meet new quality and patient protection standards. These changes aimed to improve the quality of care and protect patient choice and benefits. Today, Medicare Advantage plans continue to evolve, with an increasing focus on value-based care, telehealth services, and advanced population health management.
Importance of Medicare Advantage Plans to Beneficiaries
Medicare Advantage plans have become an essential part of the healthcare system, offering beneficiaries a range of benefits and services not always available under traditional Medicare. Some of the key advantages of Medicare Advantage plans include:
-
Coordinated care: Medicare Advantage plans often provide comprehensive, coordinated care, including preventive services, chronic disease management, and specialist care.
-
Cost savings: Many Medicare Advantage plans offer lower out-of-pocket costs, including reduced copays and deductibles, compared to traditional Medicare.
-
Enhanced benefits: Medicare Advantage plans often provide additional benefits, such as vision, dental, and hearing coverage, which are not included in traditional Medicare.
-
Broker support: Medicare beneficiaries can rely on brokers to guide them through the plan selection process, ensuring they choose a plan that suits their needs and budget.
Predictions and Estimates, 2026 bcbs medicare advantage plans
According to the Centers for Medicare and Medicaid Services (CMS), Medicare Advantage enrollment is projected to continue growing, reaching an estimated 43.4 million beneficiaries by 2026. This increase is expected to be driven by the growing population of eligible Medicare beneficiaries and the expanding range of plan options.
The growing popularity of Medicare Advantage plans highlights the continued need for these plans to adapt to the evolving healthcare landscape, focus on quality and cost, and meet the diverse needs of beneficiaries.
Prescription Drug Coverage and Formulary Changes for 2026 BCBS Medicare Advantage Plans
BCBS Medicare Advantage plans for 2026 will introduce changes in prescription drug coverage and formularies, affecting the medications available to beneficiaries. Understanding these changes is essential for individuals on Medicare to make informed decisions about their healthcare.
Changes in the Formulary for 2026 BCBS Medicare Advantage Plans
In 2026, BCBS Medicare Advantage plans will revise their formularies, adding or removing medications. Key changes include the introduction of new medications for chronic conditions like diabetes, heart disease, and cancer. Additionally, some medications will be moved to higher tiers, which may impact out-of-pocket costs.
- The introduction of newer medications for chronic conditions, such as:
- Oral medications for diabetes treatment, including newer SGLT-2 inhibitors
- Newer medications for blood pressure management, including mineralocorticoid receptor antagonists
- Immunotherapies for cancer treatment, including checkpoint inhibitors
- Movement of medications to higher tiers, resulting in:
- Increased copayments, coinsurance, or out-of-pocket costs for certain medications
Identifying Covered Medications under BCBS Medicare Advantage Plans
Beneficiaries on BCBS Medicare Advantage plans can identify covered medications using the following methods:
* Checking the BCBS Medicare Advantage Plan formulary or medication list
* Contacting the plan’s customer service or customer support
* Using online medication comparison tools or resources
* Consulting with their healthcare provider or pharmacist
Restrictions and Prior-Authorization Requirements
Some medications under BCBS Medicare Advantage plans may have restrictions or prior-authorization requirements, which are in place to ensure safe and effective use. These restrictions may include:
* Prior authorization for certain medications, requiring submission of medical records or clinical documentation
* Quantity limits or step therapy requirements
* Exclusions or limitations for certain medications
Prior authorization requirements aim to prevent unnecessary or excessive use of medications, promoting safe and effective treatment.
In 2026, BCBS Medicare Advantage plans will revise their prior-authorization requirements for certain medications, including:
* Certain medications for chronic conditions, such as opioids or benzodiazepines
* Medications with a higher risk of adverse effects or interactions
- The revised prior-authorization requirements will include:
- Shortened review periods or expedited approval processes for urgent cases
- Increased flexibility in medication management for patients with complex medical needs
Understanding the changes in prescription drug coverage and formularies for 2026 BCBS Medicare Advantage plans is essential for making informed decisions about healthcare. Beneficiaries can access covered medications, navigate restrictions and prior-authorization requirements, and ensure safe and effective treatment.
Plan Networks and Access to Care for 2026 BCBS Medicare Advantage Plans
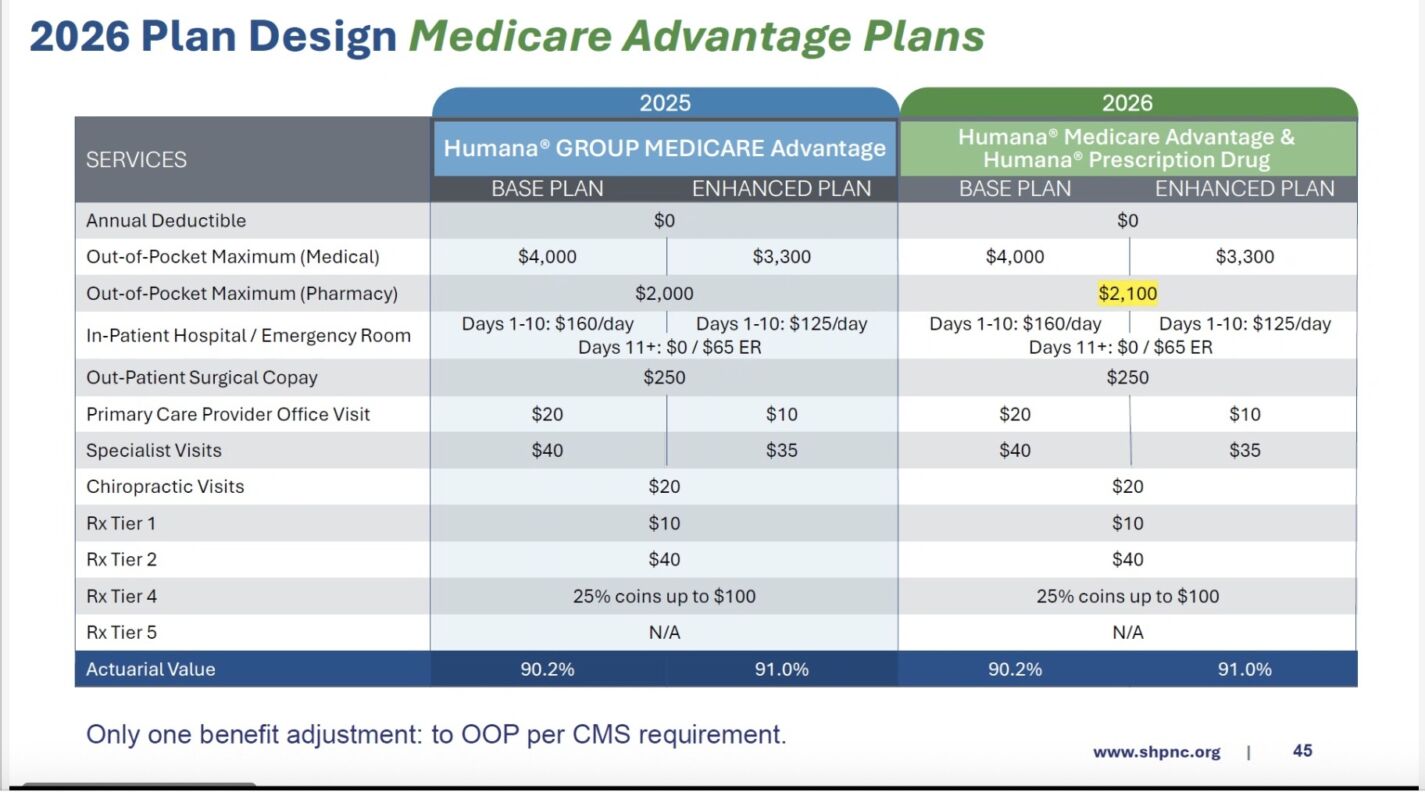
For the 2026 BCBS Medicare Advantage plans, understanding the plan networks and access to care is crucial for beneficiaries to make informed decisions about their healthcare coverage. Plan networks, also known as provider networks, refer to the group of healthcare providers, such as doctors, hospitals, and specialists, who have agreed to provide services to beneficiaries at a negotiated rate. The network size and type can significantly impact the accessibility of care and overall costs for beneficiaries.
### Types of BCBS Medicare Advantage Plan Networks
Difference between HMO, PPO, and SNP Plan Networks
There are several types of plan networks offered by BCBS Medicare Advantage plans, including Health Maintenance Organization (HMO), Preferred Provider Organization (PPO), and Special Needs Plan (SNP). Each type of network has its unique characteristics, advantages, and disadvantages.
#### HMO Plan Networks
– Limited Provider Network: Beneficiaries must receive care from providers within the plan’s network, except in emergency situations.
– Primary Care Physician (PCP) Required: Beneficiaries must designate a PCP, who coordinates their care and refers them to specialists within the network.
– No Out-of-Network Coverage: Beneficiaries are not covered for services received from out-of-network providers, except in emergency situations.
#### PPO Plan Networks
– Larger Provider Network: Beneficiaries have a broader network of providers to choose from, including both in-network and out-of-network options.
– No PCP Requirement: Beneficiaries are not required to designate a PCP, and can see any provider within or outside the network.
– Some Out-of-Network Coverage: Beneficiaries may receive some coverage for out-of-network services, but at a higher cost.
#### SNP Plan Networks
– Limited to Special Needs Beneficiaries: SNP plans are designed for beneficiaries with specific needs, such as Chronic Renal Disease or HIV/AIDS.
– Specialized Network: SNP plans have a network of providers with expertise in caring for beneficiaries with these conditions.
### Out-of-Network Services and Additional Resources
Accessing Out-of-Network Services and Additional Resources
In situations where beneficiaries need to access out-of-network services or additional resources, such as specialists or medical services not covered by their plan, there are several options available.
#### Out-of-Network Services
– Emergency Services: Beneficiaries are always covered for emergency services, regardless of the provider’s network status.
– Non-Emergency Services: Beneficiaries may be covered for non-emergency services from out-of-network providers, but at a higher cost and with prior authorization or a referral from their PCP.
– Secondary Insurance: Beneficiaries may have secondary insurance that covers out-of-network services, such as Medigap insurance.
#### Additional Resources
– PCPs and Specialists: Beneficiaries can see a specialist within or outside their plan’s network, with a referral from their PCP.
– Durable Medical Equipment (DME) and Supplies: Beneficiaries can obtain DME and supplies from out-of-network providers, but with prior authorization from their plan.
– Home Health Care and Hospice: Beneficiaries can receive home health care and hospice services from out-of-network providers, but with prior authorization and coordination of care with their PCP.
### Limitations to Access Care
Limitations to Accessing Care under BCBS Medicare Advantage Plans
While BCBS Medicare Advantage plans offer a range of benefits and services, there are also limitations to accessing care that beneficiaries should be aware of.
#### Referral Requirements
– PCP Referral Required: Beneficiaries must have a referral from their PCP to see a specialist within the plan’s network.
– Prior Authorization Required: Beneficiaries may need prior authorization from their plan or PCP for non-emergency services, such as surgeries or hospitalizations.
#### Network Rotations and Terminations
– Network Changes: BCBS Medicare Advantage plans may update their network of providers, which can limit access to care for beneficiaries.
– Terminated Providers: Providers may be terminated from the network for various reasons, such as non-compliance with plan requirements or poor quality of care.
### Conclusion
BCBS Medicare Advantage plans offer a range of benefits and services, but beneficiaries must be aware of the plan networks and access to care. Understanding the differences between HMO, PPO, and SNP plan networks, out-of-network services, and additional resources can help beneficiaries make informed decisions about their healthcare coverage. Additionally, limitations to accessing care, such as referral requirements and network rotations, should be carefully reviewed to ensure that beneficiaries have adequate access to necessary healthcare services.
Cost of 2026 BCBS Medicare Advantage Plans and Any Additional Fees

The cost of 2026 BCBS Medicare Advantage plans can be complex, with multiple factors contributing to the overall expense. Understanding these costs is essential to make informed decisions about your healthcare coverage.
Premium Costs
BCBS Medicare Advantage plans have a monthly premium that varies based on factors such as age, plan type, and location. In 2026, the average monthly premium for BCBS Medicare Advantage plans is expected to be around $50-$70. However, this cost can range from $30 to over $100 per month, depending on the specific plan and individual circumstances.
For example, let’s assume a 65-year-old individual chooses a BCBS Medicare Advantage plan with a premium of $60 per month. This means that over the course of a year, the individual would pay $720 in premiums alone.
Out-of-Pocket (OOP) Costs
In addition to monthly premiums, BCBS Medicare Advantage plans also have OOP costs, which include deductibles, copays, coinsurance, and other out-of-pocket expenses. These costs can vary significantly depending on the plan and individual circumstances.
Some common OOP costs associated with BCBS Medicare Advantage plans include:
- Deductibles: The amount an individual must pay for medical services before the plan begins to cover costs.
- Copays: A fixed amount an individual must pay for each doctor visit or prescription medication.
- Coinsurance: A percentage of medical costs that an individual must pay after meeting the deductible.
- Maximum Out-of-Pocket (MOOP): The maximum amount an individual must pay in OOP costs within a calendar year.
For example, let’s assume a BCBS Medicare Advantage plan has a deductible of $300, copays of $20 for doctor visits and $50 for prescription medications, and coinsurance rates of 20%. If the individual has a medical bill of $1,000, they would pay $200 (20% coinsurance) after meeting the deductible.
Maximum Out-of-Pocket (MOOP) Costs
The MOOP cost for BCBS Medicare Advantage plans is the maximum amount an individual must pay in OOP costs within a calendar year. This cost is usually around $3,450, but can range from $2,400 to over $6,700, depending on the plan and individual circumstances.
For example, let’s assume a BCBS Medicare Advantage plan has an MOOP cost of $3,450. If the individual incurs medical expenses totaling $10,000 within a calendar year, they would pay the first $3,450 in OOP costs and the remaining $6,550 would be covered by the plan.
Additional Fees
In addition to premiums and OOP costs, BCBS Medicare Advantage plans may also have additional fees, such as:
Late Enrollment Penalty (LEP)
Individuals who join a Medicare Advantage plan after the initial enrollment period may be subject to a LEP, which can increase their premiums.
Cancellation Fees
If an individual cancels their Medicare Advantage plan before the end of the contract year, they may be liable for cancellation fees.
Part B Premium Surcharge
Individuals who have Medicare Part B and a Medicare Advantage plan may be subject to a Part B premium surcharge, which can increase their Part B premiums.
Other Fees
Some BCBS Medicare Advantage plans may also have additional fees, such as:
- Home health care fees
- Nursing home fees
- Durable medical equipment (DME) fees
These fees can vary depending on the plan and individual circumstances.
Calculating Total Costs
To calculate the total costs of a BCBS Medicare Advantage plan, individuals should consider the following:
- Premium costs: The monthly premium and any late enrollment penalty (LEP)
- OOP costs: Deductibles, copays, coinsurance, and MOOP costs
- Additional fees: Late enrollment penalty (LEP), cancellation fees, Part B premium surcharge, and other fees
For example, let’s assume a BCBS Medicare Advantage plan has a monthly premium of $60, a deductible of $300, copays of $20 for doctor visits and $50 for prescription medications, coinsurance rates of 20%, an MOOP cost of $3,450, a LEP of $20, and a Part B premium surcharge of $10. The total annual cost for this individual would be:
$60 (premium) x 12 = $720
+ $300 (deductible)
+ $20 (copay for doctor visit) x 12 = $240
+ $50 (copay for prescription medication) x 12 = $600
+ 20% (coinsurance) x $10,000 (medical expenses) = $2,000
+ $3,450 (MOOP)
+ $20 (LEP)
+ $10 (Part B premium surcharge)
= $6,980
This example illustrates the importance of considering all costs when selecting a BCBS Medicare Advantage plan. Individuals should carefully review the plan’s details and calculate their total costs to ensure they understand the full financial implications of their choice.
Star Ratings and Quality Performance for BCBS Medicare Advantage Plans in 2026
Medicare’s star ratings system evaluates the quality of care provided by Medicare Advantage plans, including those offered by Blue Cross Blue Shield (BCBS). This system assigns a score from 1 to 5 stars to each plan, with higher ratings indicating better performance. Understanding the star ratings system is crucial for beneficiaries to make informed decisions about their health insurance coverage.
Medicare evaluates BCBS Medicare Advantage plans based on a set of quality metrics that assess various aspects of care, including health outcomes, patient experience, and process measures. The specific criteria used to evaluate quality performance include:
- Health outcomes: Measures of patients’ health status, such as blood pressure control, diabetes management, and hospital readmissions.
- Patient experience: Surveys of patients’ satisfaction with their care, including access to care, communication with healthcare providers, and ease of getting referrals.
- Process measures: Metrics that evaluate the quality of care processes, such as timeliness of care, coordination of care, and use of evidence-based treatments.
These criteria are designed to gauge the overall quality of care provided by BCBS Medicare Advantage plans and help beneficiaries compare plans based on their performance.
Examples of BCBS Medicare Advantage Plans with High Star Ratings
Some examples of BCBS Medicare Advantage plans with high star ratings include:
- The Blue Cross Blue Shield of Massachusetts HMO plan, which earned a 4.5-star rating for its strong performance in health outcomes, patient experience, and process measures.
- The Blue Cross Blue Shield of Michigan PPO plan, which received a 4.5-star rating for its high ratings in patient experience, process measures, and health outcomes.
- The Blue Cross Blue Shield of Arizona HMO plan, which earned a 4.5-star rating for its strong performance in patient experience, process measures, and health outcomes.
These plans have demonstrated a commitment to providing high-quality care, which is reflected in their star ratings. Beneficiaries should review the specific star ratings for each plan they are considering to make informed decisions about their coverage.
Making informed choices about Medicare coverage is crucial for ensuring access to high-quality care.
Medicare’s star ratings system provides valuable information to help beneficiaries navigate the complex world of Medicare Advantage plans. By understanding how quality is measured and evaluated, beneficiaries can make informed decisions about their health insurance coverage and choose a plan that meets their needs and expectations.
Choosing the Best 2026 BCBS Medicare Advantage Plan: 2026 Bcbs Medicare Advantage Plans
Selecting the most suitable BCBS Medicare Advantage plan can be a daunting task, given the numerous options available. It is essential to carefully evaluate and compare various plans to ensure that you choose the one that best meets your individual needs and health requirements. To make an informed decision, consider the following key factors when selecting a 2026 BCBS Medicare Advantage plan.
Understanding Your Health Needs
To choose the best 2026 BCBS Medicare Advantage plan, it is crucial to understand your health needs and requirements. Consider the following factors:
* Do you have any chronic health conditions requiring regular medication or treatment?
* Are you likely to need frequent doctor visits or hospitalizations?
* Do you require specialized care, such as physical therapy or mental health services?
* Are you interested in preventive care and wellness programs?
When evaluating the plans, pay attention to the coverage and benefits provided by each, including pharmacy costs, copays, coinsurance, and deductibles.
Assessing Plan Networks and Providers
Another essential factor to consider is the plan network and provider options. Ensure that your preferred healthcare providers and specialists are part of the plan’s network. This will help you maintain continuity of care and ease of access to medical services.
When reviewing plan networks, ask yourself:
* Are my regular healthcare providers part of the plan’s network?
* What is the scope of the network, including hospitals, clinics, and specialist services?
* Are there any limitations on referrals or secondary care services?
To make a more informed decision, use the following tools and resources to compare 2026 BCBS Medicare Advantage plans:
Using Comparative Tools and Resources
* The Centers for Medicare and Medicaid Services (CMS) offers the “Plan Finder” tool to compare and analyze Medicare Advantage plans.
* The Medicare website provides detailed information on plan benefits, network providers, and costs.
* Independent non-profit organizations, such as the Medicare Rights Center, offer unbiased advice and resources to help beneficiaries navigate the Medicare Advantage plan landscape.
* Consult with a licensed insurance professional or a State Health Insurance Assistance Program (SHIP) counselor for personalized guidance.
Personalized recommendations are essential when selecting a 2026 BCBS Medicare Advantage plan. Consider the following:
* Do you have a personal or family health history that may impact your plan selection?
* Are there specific health concerns or needs that would require tailored coverage?
* Do you have any mobility or transportation issues that may impact access to medical services?
Take the time to thoughtfully evaluate and compare plans, considering your unique health needs, preferences, and circumstances. This will enable you to make an informed decision and choose the best 2026 BCBS Medicare Advantage plan for you.
Ultimate Conclusion

In conclusion, 2026 bcbs medicare advantage plans offer a wide range of benefits, services, and coverage options, making it crucial to carefully consider your needs and preferences when selecting a plan. By taking the time to understand the different aspects of these plans, you can ensure that you receive the best possible care and coverage for your specific situation.
Essential FAQs
Q: What is the difference between BCBS Medicare Advantage plans and Original Medicare?
A: BCBS Medicare Advantage plans offer a range of additional benefits, services, and coverage options not available with Original Medicare. These plans are typically administered by private insurance companies, such as Blue Cross Blue Shield, and are tailored to meet the specific needs of beneficiaries.
Q: How do I qualify for BCBS Medicare Advantage plans?
A: To qualify for BCBS Medicare Advantage plans, you must be enrolled in Medicare Part A and Part B, and meet the specific eligibility requirements set by the plan. These requirements may include age, income level, and residency status.
Q: Can I change my BCBS Medicare Advantage plan during the year?
A: Depending on your circumstances, you may be able to make changes to your BCBS Medicare Advantage plan during the year. These changes may be subject to enrollment deadlines and specific requirements, so it’s essential to review your plan documents and consult with the plan administrators.
Q: How do I compare BCBS Medicare Advantage plans?
A: To compare BCBS Medicare Advantage plans, consider factors such as premium costs, coverage options, network providers, and prescription drug coverage. You can also use online tools and resources to compare plans and receive personalized recommendations.