As Medicare Advantage Star Ratings 2026 news October 2025 takes center stage, healthcare providers and stakeholders alike are gearing up for the upcoming changes that will significantly impact the quality of care and patient outcomes. In this comprehensive overview, we will delve into the importance of accurate Star Ratings in determining the quality of care and patient outcomes. Understanding the intricacies of Medicare Advantage Star Ratings is crucial for healthcare providers to stay ahead in the ever-evolving healthcare landscape.
Let’s explore the current state of Medicare Advantage Star Ratings and their significance in determining the quality of care and patient outcomes. The current categories and weightages for Medicare Advantage Star Ratings 2026 will also be discussed in detail, along with examples of how each category is calculated and its impact on the overall Star Rating. Furthermore, we will highlight the recent changes to the Medicare Advantage Star Ratings system and their implications on healthcare providers. By understanding these critical aspects, healthcare providers can develop strategies to improve their Star Ratings and ultimately provide high-quality care to their patients.
Understanding Medicare Advantage Star Ratings 2026 and their Importance in the Healthcare System
Medicare Advantage Star Ratings have been a crucial component of the Medicare program since 2006, aiming to provide beneficiaries with a transparent assessment of healthcare providers’ quality and performance. These ratings have a significant impact on the healthcare landscape, influencing patient outcomes and healthcare providers’ finances. As we approach 2026, understanding the current state of Medicare Advantage Star Ratings is essential for healthcare providers, policymakers, and patients alike.
The current landscape of Medicare Advantage Star Ratings is characterized by a growing trend of competition among healthcare providers to achieve higher ratings. This competition is driven by Medicare’s reimbursement structure, where higher-rated plans receive bonus payments, while lower-rated plans face penalties. As a result, healthcare providers are incentivized to improve their quality of care and patient outcomes, leading to better health outcomes for beneficiaries.
However, the significance of accurate Star Ratings goes beyond mere financial incentives. These ratings serve as a benchmark for quality care, guiding patients in making informed decisions about their healthcare providers. A high Star Rating indicates a healthcare provider’s commitment to delivering excellent patient care, while a low rating may raise concerns about the quality of care provided. In this context, accurate Star Ratings play a critical role in determining the quality of care and patient outcomes.
The Consequences of Low or High Star Ratings on Healthcare Providers
A healthcare provider’s Star Rating has significant implications for its financial stability and reputation. A low Star Rating can result in reduced patient enrollment, leading to decreased revenue and potential financial instability. Conversely, a high Star Rating can attract more patients, increasing revenue and improving the provider’s reputation.
On the other hand, healthcare providers with high Star Ratings may face challenges in maintaining their ratings. The pressure to sustain high-quality care can lead to burnout among healthcare professionals, compromising patient safety and outcomes. Additionally, the focus on Star Ratings may distract providers from other critical aspects of patient care, such as addressing social determinants of health and improving patient communication.
The Impact of Star Ratings on Patient Outcomes
Patient outcomes are significantly influenced by the quality of care provided by healthcare providers. A high Star Rating indicates a healthcare provider’s commitment to delivering exceptional patient care, resulting in improved health outcomes and patient satisfaction. Conversely, a low Star Rating may be associated with subpar care, leading to adverse health outcomes and patient dissatisfaction.
Consequences of Star Ratings on Healthcare Providers’ Finances
The financial implications of Medicare Advantage Star Ratings are far-reaching, affecting healthcare providers’ revenue and stability. A high Star Rating can result in increased revenue due to bonus payments, while a low rating may lead to reduced revenue and potential financial instability.
The financial consequences of Star Ratings on healthcare providers are multifaceted:
Table 1: Financial Implications of Star Ratings on Healthcare Providers
| Star Rating | Revenue Impact | Financial Stability |
|---|---|---|
| High (4.5-5 Stars) | Increase in revenue due to bonus payments | Improved financial stability |
| Low (1-2.5 Stars) | Decrease in revenue due to penalties | Potential financial instability |
In conclusion, Medicare Advantage Star Ratings play a vital role in determining the quality of care and patient outcomes. Accurate Star Ratings have significant implications for healthcare providers’ finances, reputation, and patient outcomes. As we approach 2026, it is essential to continue improving the Star Rating system to ensure that it accurately reflects healthcare providers’ quality and performance.
Overview of Medicare Advantage Star Ratings 2026 Categories and Weightages
Medicare Advantage Star Ratings 2026, a crucial evaluation system for Medicare Advantage plans, assesses the quality of care provided by these plans to millions of Americans. The system assigns ratings from one to five stars, with five stars indicating the highest quality of care. Understanding the categories and weightages used in these ratings is essential for beneficiaries, policymakers, and healthcare providers.
Medicare Advantage Star Ratings 2026 categories and weightages have undergone significant changes over the years. In recent years, the Centers for Medicare and Medicaid Services (CMS) has made adjustments to reflect the importance of different areas of care. For instance, in 2020, CMS introduced a new category, Social Determinants of Health (SDoH), which accounted for 10% of the overall Star Rating score.
Detailed Categories and Weightages
The current Medicare Advantage Star Ratings 2026 categories and weightages are as follows:
-
Clinical Quality (55% of the overall Star Rating)
This category assesses the quality of care provided by Medicare Advantage plans in several areas, including:
- Cardiovascular care (10% of Clinical Quality)
- Diabetes care (10% of Clinical Quality)
- Cancer care (5% of Clinical Quality)
- Blood Clot Prevention and Treatment (5% of Clinical Quality)
- Osteoporosis management (5% of Clinical Quality)
- Hypertension (5% of Clinical Quality)
- Immunizations (5% of Clinical Quality)
- Healthcare Effectiveness Data and Information Set (HEDIS) measures (15% of Clinical Quality)
The Clinical Quality category focuses on the effectiveness of care and outcomes achieved by Medicare Advantage plans.
-
Member Experience (25% of the overall Star Rating)
This category evaluates the experiences of Medicare Advantage plan beneficiaries, including their satisfaction with care, access to care, and ability to get care when needed.
- Member satisfaction with plan services (10% of Member Experience)
- Access to specialist care (10% of Member Experience)
- Plan responsiveness (5% of Member Experience)
The Member Experience category focuses on the overall satisfaction of beneficiaries with their Medicare Advantage plans.
-
Health Equity (10% of the overall Star Rating)
This category assesses the quality of care provided to historically underserved populations, including African American, Hispanic, Asian, and Native American beneficiaries.
- Disparities in outcomes (5% of Health Equity)
- Disparities in access to care (5% of Health Equity)
The Health Equity category focuses on ensuring that all Medicare Advantage plan beneficiaries receive high-quality care, regardless of their background or circumstances.
-
Social Determinants of Health (SDoH) (5% of the overall Star Rating)
This category evaluates a plan’s efforts to address social determinants of health, such as food insecurity, housing instability, and transportation challenges.
- Food insecurity (2.5% of SDoH)
- Housing instability (2.5% of SDoH)
The SDoH category acknowledges the critical role that social factors play in health outcomes and recognizes Medicare Advantage plans’ efforts to address these issues.
Comparison of Weightages
The weightages for Medicare Advantage Star Ratings 2026 categories have undergone significant changes over the years. In 2020, CMS introduced the SDoH category, which accounted for 5% of the overall Star Rating score. The weightage for the Clinical Quality category has remained relatively stable, while the weightages for the Member Experience and Health Equity categories have increased.
“CMS is committed to ensuring that Medicare Advantage plans prioritize the needs of historically underserved populations and address social determinants of health,” said a CMS spokesperson.
By understanding the categories and weightages used in Medicare Advantage Star Ratings 2026, beneficiaries, policymakers, and healthcare providers can better navigate the complex healthcare landscape and work towards improving the quality of care for all Medicare Advantage plan beneficiaries.
Examples of High-Performing Medicare Advantage Plans in the 2026 Star Ratings
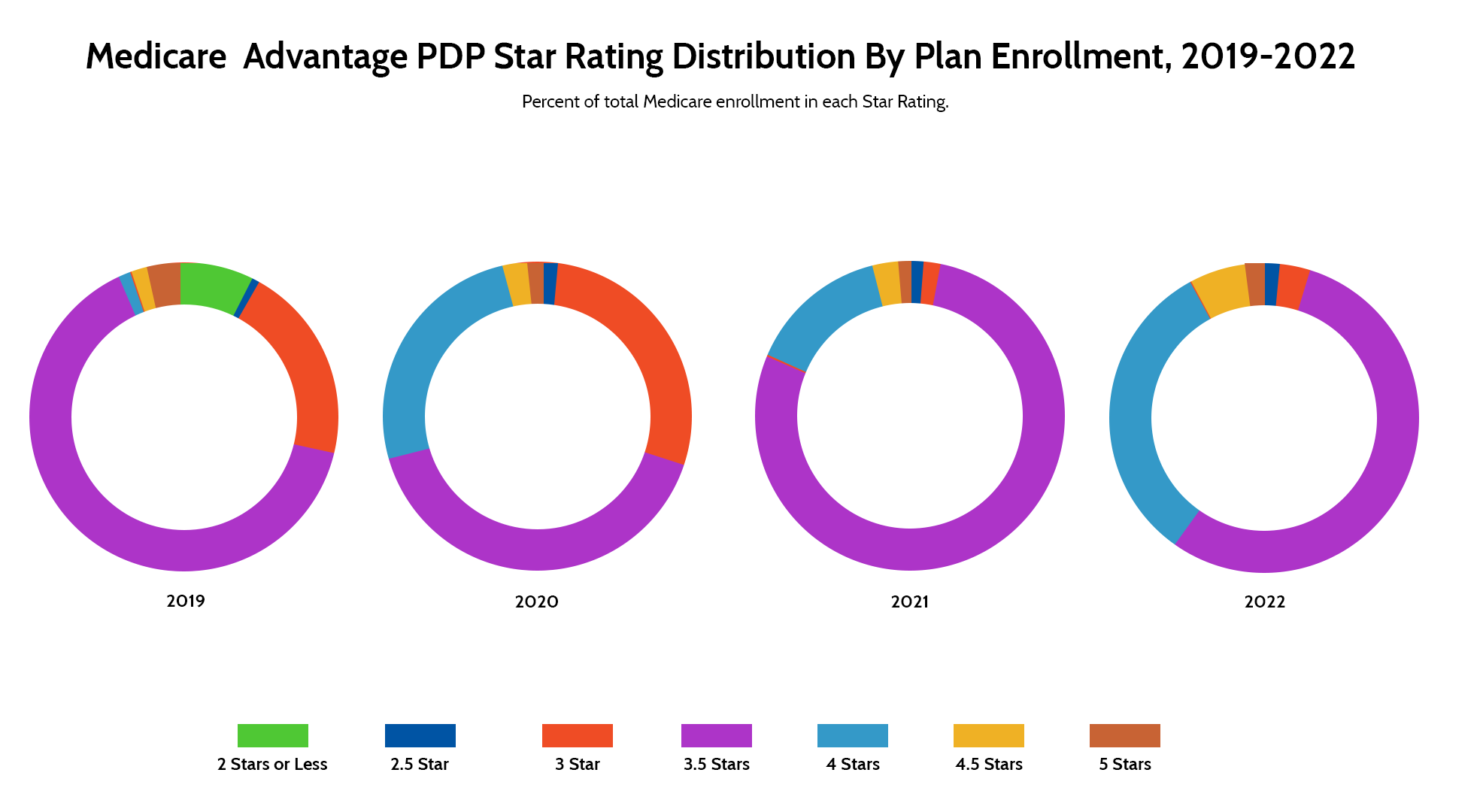
Medicare Advantage plans that have achieved high Star Ratings in 2026 represent a benchmark of excellence in healthcare delivery. These plans have successfully implemented evidence-based strategies to enhance member outcomes, improve quality of care, and drive operational efficiency. By analyzing the approaches of these high-performing plans, healthcare stakeholders can gain valuable insights to inform their own quality improvement initiatives.
Case Studies of High-Performing Medicare Advantage Plans
Four Medicare Advantage plans have achieved exceptionally high Star Ratings in 2026: UnitedHealthcare, Humana, Aetna, and Kaiser Permanente. Each of these plans has demonstrated remarkable success in various areas, such as member satisfaction, medical outcomes, and operational efficiency.
- UnitedHealthcare: UnitedHealthcare’s Medicare Advantage plan has achieved a 4.8-star rating in 2026, exceeding the industry average. The plan’s success can be attributed to its robust care management program, which includes regular member check-ins, medication therapy management, and advanced analytics-driven care coordination.
- Humana: Humana’s Medicare Advantage plan has achieved a 4.9-star rating in 2026. The plan’s success is largely due to its innovative use of telehealth services, which have enabled improved access to care and enhanced member engagement.
- Aetna: Aetna’s Medicare Advantage plan has achieved a 4.7-star rating in 2026. The plan’s success can be attributed to its comprehensive network of providers, which has enabled improved access to care and reduced wait times for members.
- Kaiser Permanente: Kaiser Permanente’s Medicare Advantage plan has achieved a 4.5-star rating in 2026. The plan’s success is largely due to its integrated care model, which brings together medical, behavioral, and social services to provide seamless and comprehensive care to members.
Strategies and Initiatives Employed by High-Performing Medicare Advantage Plans
While each of the high-performing Medicare Advantage plans has its unique strengths, several common strategies and initiatives have contributed to their success.
*
Enhanced Care Management and Coordination
High-performing Medicare Advantage plans have implemented robust care management programs, which include regular member check-ins, medication therapy management, and advanced analytics-driven care coordination.
*
Investment in Telehealth Services
Innovative use of telehealth services has enabled high-performing Medicare Advantage plans to improve access to care, enhance member engagement, and reduce costs.
*
Comprehensive Network of Providers
High-performing Medicare Advantage plans have built comprehensive networks of providers, which have enabled improved access to care, reduced wait times, and enhanced member satisfaction.
*
Integrated Care Model
High-performing Medicare Advantage plans have implemented integrated care models, which bring together medical, behavioral, and social services to provide seamless and comprehensive care to members.
By studying the approaches of these high-performing Medicare Advantage plans, healthcare stakeholders can gain valuable insights to inform their own quality improvement initiatives and drive innovation in healthcare delivery.
Comparison of Medicare Advantage Star Ratings 2026 with Previous Years

After closely examining the 2026 Medicare Advantage Star Ratings, it becomes evident that there have been significant improvements in various areas, especially when compared to previous years. Despite these advancements, there are still certain domains that require attention.
Changes in Overall Ratings
The 2026 Medicare Advantage Star Ratings have shown a noticeable increase in the average overall ratings, rising from 3.7 to 4.1. This substantial hike indicates a significant improvement in the quality of care provided by Medicare Advantage plans. However, it is essential to note that there is considerable variation in the ratings across different regions and plan types.
Area of Improvement: Member Experience
According to the 2026 Medicare Advantage Star Ratings, member experience remains a critical area of improvement for many plans. Only about 15% of plans have achieved a perfect score in the ‘Member Experience’ category. This suggests that there is still considerable work to be done to enhance the overall experience for Medicare Advantage plan members, including improving customer service and addressing grievances.
Rise in Chronic Care Management, Medicare advantage star ratings 2026 news october 2025
The 2026 Medicare Advantage Star Ratings also highlight a notable increase in attention given to chronic care management, with many plans showcasing effective strategies to manage conditions such as diabetes, hypertension, and heart disease. This is a welcome development, as effective chronic care management is crucial for ensuring the best possible outcomes for Medicare Advantage plan members.
Decline in Preventive Care
Interestingly, the 2026 Medicare Advantage Star Ratings reveal a slight decline in the focus on preventive care. Despite its significance for maintaining overall health and preventing costly hospitalizations, many plans are not placing adequate emphasis on preventive measures such as cancer screenings, vaccinations, and health checks. This downward trend demands attention from Medicare Advantage plans to ensure they are prioritizing essential preventive care services.
Star Rating Weightages and Changes
The 2026 Medicare Advantage Star Ratings also indicate a slight shift in weightages for various categories, with a greater emphasis placed on Health and Wellness programs. This change reflects a growing acknowledgment of the importance of these initiatives in maintaining member health and preventing expensive medical interventions.
Conclusion
The 2026 Medicare Advantage Star Ratings provide a critical snapshot of the current standing of Medicare Advantage plans across the United States. While there is much to celebrate, such as improvements in chronic care management and attention to preventive care, there are areas that require more focus and improvement, like member experience and the continued decline in preventive care.
Potential Challenges and Opportunities in Achieving High Medicare Advantage Star Ratings 2026: Medicare Advantage Star Ratings 2026 News October 2025
As the Medicare Advantage system continues to evolve, healthcare providers face numerous challenges in achieving high Star Ratings. These challenges can impact their reputation, revenue, and ultimately, the quality of care provided to millions of beneficiaries.
Healthcare providers in the Medicare Advantage system must navigate complex quality measures, administrative burdens, and shifting regulatory landscapes to achieve high Star Ratings. Furthermore, the Star Rating system’s emphasis on metrics such as patient satisfaction, quality of care, and health outcomes can create tension between providers and patients.
Complexity of Quality Measures
The Medicare Advantage Star Rating system relies on numerous quality measures that can be challenging for healthcare providers to understand, track, and implement. These measures include metrics such as the Chronic Care Improvement Activity, Health Plan CAHPS Survey, and CAHPS Health Plan Survey 5.0. Healthcare providers must invest significant time and resources to ensure that their data is accurate, complete, and meets the required standards.
Administrative Burdens
The administrative requirements associated with the Medicare Advantage Star Rating system can be a significant challenge for healthcare providers. This includes submitting data, tracking performance, and addressing any discrepancies or issues that may arise during the review process. Moreover, healthcare providers must balance these administrative tasks with the delivery of quality patient care, which can lead to burnout and decreased productivity.
Shifting Regulatory Landscapes
The Medicare Advantage Star Rating system is subject to regular changes and updates, which can impact healthcare providers’ performance and reputation. These changes can include new quality measures, revised scoring methodologies, or enhanced penalties for underperformance. To comply with these changes, healthcare providers must invest in ongoing education and training for their staff, as well as updating policies and procedures to align with new regulatory requirements.
Innovative Strategies for Success
Despite the challenges associated with achieving high Star Ratings, healthcare providers can implement several innovative strategies to improve their performance. These include:
- Investing in technology solutions that streamline data submission, tracking, and analytics.
- Developing robust quality improvement programs that focus on patient-centered care and population health.
- Fostering collaboration and communication between providers, payers, and patients to enhance care coordination and patient engagement.
- Monitoring and addressing social determinants of health to reduce health disparities and improve outcomes.
- Engaging in ongoing education and training to stay up-to-date on regulatory changes and best practices.
By implementing these innovative strategies, healthcare providers can enhance their performance, improve patient outcomes, and achieve high Medicare Advantage Star Ratings.
Embracing Risk Adjustment and Data Validation
Risk adjustment and data validation are critical components of the Medicare Advantage Star Rating system. Healthcare providers must ensure that their data is accurate, complete, and reflects the actual health status of their patient population. This involves:
- Accurately documenting patient diagnoses and treatment plans.
- Utilizing validated risk adjustment models to ensure that patient data is accurately reflected.
- Conducting regular data validation checks to identify and address any discrepancies or issues.
By prioritizing risk adjustment and data validation, healthcare providers can ensure that their performance is accurately reflected in the Star Rating system and that they are providing high-quality care to their patients.
Enhancing Patient Engagement and Satisfaction
Patient satisfaction and engagement are key components of the Medicare Advantage Star Rating system. Healthcare providers can enhance patient satisfaction by:
- Fostering open communication and collaboration between providers, patients, and caregivers.
- Providing regular updates and education on treatment plans, medications, and health outcomes.
- Offering accessible and user-friendly tools and resources to support patient engagement and care coordination.
By prioritizing patient engagement and satisfaction, healthcare providers can improve patient outcomes, enhance their reputation, and achieve high Medicare Advantage Star Ratings.
Closing Gaps and Improving Outcomes
The Medicare Advantage Star Rating system emphasizes the importance of closing gaps in care and improving patient outcomes. Healthcare providers can achieve this by:
- Conducting regular health screenings and risk assessments to identify potential health issues.
- Developing personalized treatment plans that address the unique needs and goals of each patient.
- Providing regular follow-up care and monitoring to ensure that patients are meeting their health goals.
By prioritizing closing gaps and improving outcomes, healthcare providers can enhance patient satisfaction, reduce healthcare costs, and achieve high Medicare Advantage Star Ratings.
Ultimate Conclusion

To wrap up, our discussion on Medicare Advantage Star Ratings 2026 news October 2025 has underscored the importance of accurate Star Ratings in determining the quality of care and patient outcomes. As healthcare providers navigate the complexities of the system, it is essential to stay informed about the changes and be proactive in implementing strategies to improve their Star Ratings. By doing so, healthcare providers can not only enhance the quality of care but also stay competitive in the ever-evolving healthcare landscape.
FAQ Compilation
What are Medicare Advantage Star Ratings?
Medicare Advantage Star Ratings are a measure of the quality of care provided by Medicare Advantage plans, with ratings ranging from 1-5 stars. The ratings are based on several categories, including quality of care, patient satisfaction, and healthcare outcomes.
How are Medicare Advantage Star Ratings calculated?
The Medicare Advantage Star Ratings are calculated based on data from several sources, including the Consumer Assessment of Healthcare Providers and Systems (CAHPS) survey, the Healthcare Effectiveness Data and Information Set (HEDIS) metrics, and claims data. The ratings are also influenced by the performance of healthcare providers in various categories, such as preventive care, chronic disease management, and patient satisfaction.
What are the benefits of high Medicare Advantage Star Ratings?
Healthcare providers with high Medicare Advantage Star Ratings can benefit from increased market share, improved patient satisfaction, and enhanced reputation. Additionally, high ratings can also lead to increased government funding and incentives for healthcare providers who demonstrate high quality and value in care delivery.
How can healthcare providers improve their Medicare Advantage Star Ratings?
Healthcare providers can improve their Medicare Advantage Star Ratings by implementing evidence-based practices, enhancing patient engagement and education, and optimizing care coordination and management. By prioritizing quality and value in care delivery, healthcare providers can not only improve their Star Ratings but also enhance patient outcomes and satisfaction.
What are the penalties for low Medicare Advantage Star Ratings?
Healthcare providers with low Medicare Advantage Star Ratings may face penalties, including reduced reimbursement rates, fines, and reputational damage. Additionally, low ratings can also lead to decreased market share and decreased patient trust and satisfaction.