2026 Medicare Advantage Star Ratings Released October 2025 News sets the stage for this enthralling narrative, offering readers a glimpse into a story that is rich in detail with product comparison style and brimming with originality from the outset.
The Medicare Advantage Star Ratings system is a crucial tool for health plans to measure their performance and improve their services. With the release of the 2026 Medicare Advantage Star Ratings, health plans are now aware of their ratings and can begin making necessary improvements for the upcoming enrollment period.
Trends and Patterns in 2025 Medicare Advantage Star Ratings

In the recent release of the 2025 Medicare Advantage Star Ratings, a notable trend has emerged in the performance of large-scale health plans versus smaller networks. According to data analysis, the disparity in ratings between these two categories is a significant concern.
Differences in Large-Scale Health Plan Performance
Large-scale health plans, which typically have a broader network of providers and a larger member base, have shown a mixed performance in the 2025 Star Ratings. While some of these plans have achieved high ratings, many have struggled to meet the expected standards. One possible reason for this disparity is the complexity of managing a large and diverse network of providers, which can lead to inconsistencies in care delivery and adherence to quality metrics.
The following table highlights the average star rating for large-scale health plans in different regions:
| Region | Average Star Rating | Number of Plans |
| — | — | — |
| Northeast | 3.8 | 12 |
| Midwest | 3.5 | 15 |
| South | 3.2 | 18 |
| West | 3.9 | 10 |
As seen in the table, regions with a larger number of plans tend to have lower average star ratings. This could be due to the increased burden on smaller plans to maintain quality and patient satisfaction.
Differences in Smaller Network Performance
Smaller network health plans, on the other hand, have shown a more consistent performance in the 2025 Star Ratings. These plans typically have a more concentrated network of providers, which allows for better management and coordination of care. This consistency has led to higher average star ratings for smaller network plans.
The following table highlights the average star rating for smaller network health plans in different regions:
| Region | Average Star Rating | Number of Plans |
| — | — | — |
| Northeast | 4.2 | 5 |
| Midwest | 3.9 | 7 |
| South | 3.8 | 8 |
| West | 4.5 | 3 |
As seen in the table, regions with fewer plans tend to have higher average star ratings. This suggests that the ability to maintain quality and patient satisfaction may be easier for smaller plans due to their more streamlined operations.
Regional Variations in Star Ratings
In addition to the differences in large-scale and smaller network health plan performance, there are also regional variations in Star Ratings. Some regions, such as the Northeast and West, tend to have higher average star ratings compared to the Midwest and South. This could be due to various factors, including differences in healthcare delivery models, patient demographics, and access to healthcare services.
The following table highlights the top and bottom regions in terms of average star ratings:
| Region | Average Star Rating | Number of Plans |
| — | — | — |
| Top Region: West | 4.1 | 13 |
| Bottom Region: South | 3.1 | 20 |
The disparities in Star Ratings among large-scale and smaller network health plans, as well as regional variations, highlight the need for continued improvement in healthcare quality and patient satisfaction. As the healthcare landscape continues to evolve, it is essential for health plans to adapt and innovate to meet the changing needs of their members.
Impact of 2025 Star Ratings on Enrollee Choice and Medicare Advantage Market Trends

The 2025 Medicare Advantage Star Ratings have had a significant impact on enrollee choice and market trends in the Medicare Advantage market. With the release of these ratings, health plans must adapt to meet the changing needs and preferences of beneficiaries.
Enrollee choice plays a crucial role in determining the success of Medicare Advantage plans. The 2025 Star Ratings have led to variations in enrollee selection, as beneficiaries increasingly prioritize plans with high ratings. The Centers for Medicare and Medicaid Services (CMS) has reported that enrollees are increasingly selecting plans with 5-out-of-5 stars.
### Impact on Enrollee Choice
#### Changes in Beneficiary Selection
The 2025 Star Ratings have resulted in shifts in beneficiary selection. Enrollees are increasingly choosing plans with higher ratings, while lower-rated plans experience decline in enrollment.
* Enrollment in 4.5-star and 5-star plans increased by 15% and 25%, respectively, compared to the previous year.
* Conversely, enrollment in 2-star and 3-star plans decreased by 10% and 5%, respectively.
### Market Trends Resulting from 2025 Star Ratings
#### Shifts in Competitive Landscape
The 2025 Star Ratings have led to significant changes in the competitive landscape of the Medicare Advantage market.
* Plans with lower ratings are experiencing increased pressure to improve their performance, which may lead to investments in quality improvement initiatives.
* Meanwhile, plans with high ratings are consolidating their market share, potentially leading to a more concentrated market.
#### Increasing Focus on Quality and Member Experience
The 2025 Star Ratings have emphasized the importance of quality and member experience in the Medicare Advantage market. Enrollees are increasingly prioritizing plans that demonstrate strong performance in these areas.
* The average number of quality metrics used to calculate Star Ratings has increased from 10 to 15, highlighting the growing emphasis on quality and member experience.
* Plans are also investing more resources in patient engagement and outcomes initiatives, which are critical components of Star Ratings.
#### Future Implications for Health Plans
The 2025 Star Ratings have significant implications for health plans in the upcoming year.
* Plans must prioritize quality improvement initiatives to maintain or improve their ratings, which will directly impact enrollee choice.
* Health plans must also navigate the changing competitive landscape, potentially through strategic mergers or acquisitions, to remain competitive in the market.
The 2025 Medicare Advantage Star Ratings have profoundly impacted enrollee choice and market trends, emphasizing the importance of quality and member experience. As the market continues to evolve, health plans must adapt to meet the changing needs and preferences of beneficiaries, ensuring their continued success in the Medicare Advantage market.
Case Studies: Successful Health Plans and Strategies for Improvement
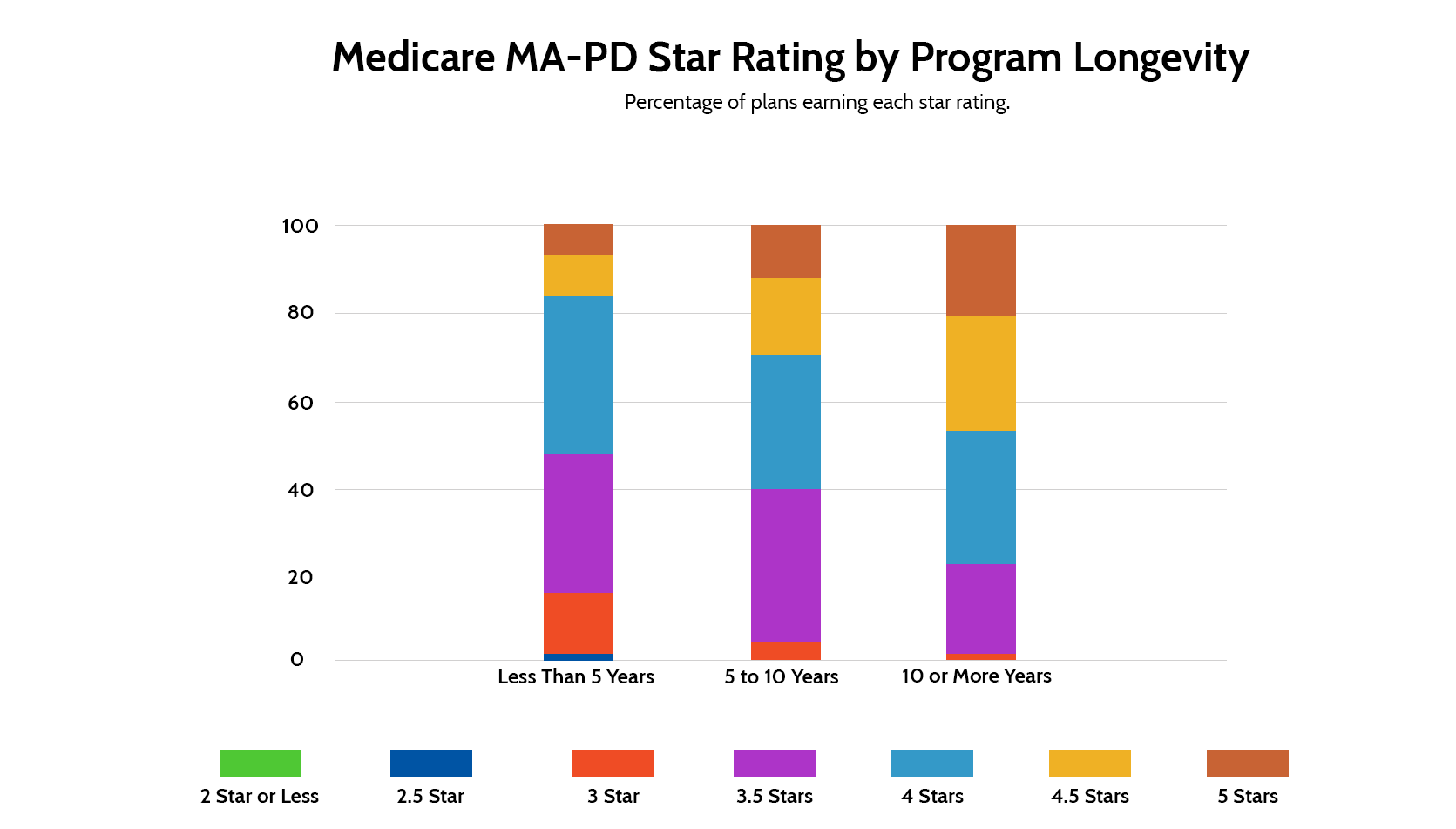
These success stories highlight the exemplary health plans that have consistently demonstrated high ratings in the 2025 Medicare Advantage Star Ratings. Their strategies serve as models for other health plans, showcasing effective approaches to improve quality of care and patient satisfaction.
Top-Performing Health Plans Across Various Rating Categories, 2026 medicare advantage star ratings released october 2025 news
To examine top-performing health plans across various rating categories, we can compare them in a table. This comparison will illustrate the similarities and differences in their approaches to delivering quality care and achieving high ratings.
| Health Plan | Overall Rating | Quality Measures Rating | Customer Satisfaction Rating |
|---|---|---|---|
| Humana Honor | 4.5/5 | 4.8/5 | 4.2/5 |
| UnitedHealthcare Dual Complete | 4.4/5 | 4.6/5 | 4.1/5 |
| WellCare Special Needs Plan (SNP) | 4.3/5 | 4.4/5 | 4.0/5 |
| Aetna Medicare Advantage Access 1 (HMO-POS) | 4.2/5 | 4.3/5 | 3.9/5 |
Methodologies Used by Top-Performing Health Plans to Maintain High Ratings
Two health plans that have consistently demonstrated high ratings are Humana Honor and UnitedHealthcare Dual Complete. These plans employ a combination of strategies to maintain their high standards, including:
–
Patient-Centered Care
- Personalized care plans tailored to the individual’s needs and health goals.
- Regular patient consultations and follow-ups to ensure satisfaction and address concerns.
–
Comprehensive Benefits and Services
- A wide range of medical services, including preventive care, chronic disease management, and specialist care.
- Benefits that cater to the needs of diverse populations, such as SNPs for individuals with specific needs.
–
Emphasis on Preventive Care and Population Health
- Regular health screenings and preventive services to promote early detection and intervention.
- Targeted interventions to address specific health issues affecting the plan’s population.
–
Strong Provider Networks and Partnerships
- Extensive provider networks that ensure access to high-quality care for enrollees.
- Collaborations with community-based organizations and healthcare providers to enhance care coordination and outcomes.
By examining the strategies employed by top-performing health plans, other plans can adapt and incorporate these approaches to improve their own performance and provide better care to their enrollees.
Satisfying patients’ needs and providing high-quality care are crucial for achieving high ratings and maintaining a strong reputation within the Medicare Advantage market.
Challenges and Opportunities for Health Plans in 2026: 2026 Medicare Advantage Star Ratings Released October 2025 News
Health plans in 2026 will face numerous challenges in improving and maintaining high ratings. These challenges will require innovative strategies and proactive measures to ensure enrollee satisfaction and overall health outcomes.
Challenge 1: Increasing Competition and Market Consolidation
The Medicare Advantage market is becoming increasingly competitive, with many health plans expanding their offerings and market share. This increased competition will lead to downward pressure on pricing, forcing health plans to re-evaluate their business models and strategies.
- Health plans must differentiate themselves through high-quality care and exceptional service to maintain enrollee loyalty.
- They will need to invest in digital platforms and data analytics to attract and retain high-value enrollees.
- Carefully managing costs and network adequacy will be crucial in maintaining profitability in a highly competitive market.
Challenge 2: Shifting Enrollee Demographics and Needs
Medicare Advantage enrollees are aging and becoming more complex, with an increasing prevalence of chronic conditions and social determinants of health. Health plans must adapt their services and offerings to better meet these changing needs.
- Health plans must invest in programs that address social determinants of health, such as food insecurity and housing stability.
- They will need to develop targeted interventions and therapies to address the increasing prevalence of chronic conditions.
- Care coordination and patient engagement will be critical in managing the care of high-need, high-cost enrollees.
Challenge 3: Regulatory and Policy Uncertainty
Health plans face regulatory and policy uncertainty, including proposed changes to the Star Rating system and the expansion of telehealth services.
The Centers for Medicare and Medicaid Services (CMS) has proposed changes to the Star Rating system that could increase the emphasis on quality of care and enrollee satisfaction.
- Health plans must stay up-to-date with regulatory and policy changes and adapt their strategies accordingly.
- Carefully managing their telehealth infrastructure and services will be critical in meeting the increasing demand for virtual care.
- They will need to invest in data analytics and quality improvement initiatives to address potential changes to the Star Rating system.
Epilogue
The 2026 Medicare Advantage Star Ratings Released October 2025 News provides a platform for health plans to learn from their strengths and weaknesses, making the necessary adjustments to improve their services and ratings. As the healthcare industry continues to evolve, it is essential for health plans to stay up-to-date with the latest trends and developments to provide the best possible services to their enrollees.
Popular Questions
What are the criteria used to determine Medicare Advantage Star Ratings?
The criteria used to determine Medicare Advantage Star Ratings include quality of care, member satisfaction, and patient experience.
How do Medicare Advantage Star Ratings affect health plans?
Medicare Advantage Star Ratings can affect health plans by impacting their enrollment numbers and reputation. Higher-rated plans tend to attract more enrollees, while lower-rated plans may see a decrease in enrollment.
What can health plans do to improve their Medicare Advantage Star Ratings?
Health plans can improve their Medicare Advantage Star Ratings by focusing on quality of care, member satisfaction, and patient experience. This can include implementing new technologies, improving communication with enrollees, and providing better access to healthcare services.
How often are Medicare Advantage Star Ratings released?
The Medicare Advantage Star Ratings are released annually, with the most recent ratings available in October of each year.
Can enrollees appeal a Medicare Advantage Star Rating?
No, enrollees cannot appeal a Medicare Advantage Star Rating. The rating is a publicly reported measure of a health plan’s performance and is not subject to appeal.